Also known as pityriasis versicolor, tinea versicolor is a specific kind of fungal skin infection that is identified by an anomalous skin rash. It is caused due to proliferation of a species of yeast which is naturally found on human skin.
The usual pigmentation of skin is adversely affected by tinea versicolor-causing yeast overgrowth leading to the appearance of small discolored blotches on the skin. These abnormal patches on the skin are a shade lighter or darker than the surrounding areas.
The torso and shoulders are most commonly affected by tinea versicolor. Teenagers and young adults are more susceptible to the infection than others. The abnormal skin rashes may become more noticeable after contact with sunlight.
Tinea versicolor is treated with topical antifungal medications. The discoloration may however continue for several weeks even after a successful cure. Patients may also suffer from a relapse under the right conditions of warm and humid weather.
Symptoms of tinea versicolor
Uncontrolled growth of the causative fungus prevents the body from effectively dealing with the acidic bleach secreted by the yeast. This is what causes the infected skin to turn darker or lighter than the adjacent areas. The skin rashes can occur in groups or as a single anomalous spot.
Listed below are a few usual signs and symptoms of tinea versicolor:
- Appearance of discolored spots on skin. Such abnormal patches may be white, brown, pink, or red in color. They usually have a lighter or darker hue as compared to nearby skin.
- The spots often disappear in cooler weather, but can aggravate or make a reappearance in warm and humid conditions.
- Some patients may experience itching and discomfort, or scaling or dryness of the patches.
- Tinea versicolor affected skin does not tan like the skin regions unaffected by the fungal infection.
- The abnormal patches can occur anywhere on the body, but are predominantly found on the neck, chest, back, and arms.
Causes of tinea versicolor
Tinea versicolor is caused due to uncontrolled and rapid growth of a yeast/fungus that is found to naturally live on human skin. There are several factors which can contribute towards proliferation of the fungus, the most common of which are listed below:
- People with oily skin are more prone to developing tinea versicolor.
- People living in a tropical region with hot and humid climate are at greater risk.
- Excessive sweating increases the risk.
- People with a weakened immune system are also more vulnerable.
The causal fungus naturally occurs on human skin and hence tinea versicolor is not contagious. Teenagers and adults in their 20s and 30s are more prone to developing tinea versicolor.People of all races and skin colors can suffer from this infection.
Diagnosis
- Doctors can diagnose tinea versicolor just by looking at the abnormal patches.Occasionally, they may check the spots under UV light as it causes the infected skin to appear florescent yellowish-green.
- Doctors may clear any doubts via microscopic examination of affected skin and scales gathered by scraping them off from the infected areas. In the case of children, the physician may collect the specimen skin cells by attaching a clear tape on the patches and then removing it. The sample is then examined in a lab.
Treatment of tinea versicolor
Tinea versicolor infections are treated with oral and topical drugs. The method and range of treatment is devised as per the size, site, and thickness of the infected skin areas.
A few common ways to treat tinea versicolor are listed below:
- Use of anti-fungal shampoos, lotions, creams, foam, or soaps:Application of different forms of topical anti-fungal medications can help manage the growth of the yeast. Over the counter anti-fungal creams containing terbinafine, miconazole, clotrimazole, selenium sulfide, zinc, and pyrithione are commonly used. In rare instances, doctors may opt for prescription topical anti-fungal drugs.
- Use of oral anti-fungal drugs: Recurring or serious cases of tinea versicolor require treatment with anti-fungal pills. Doctors may also prescribe them for fast and simple resolution from tinea versicolor. Such prescription drugs can however cause severe side effects.
All instances of tinea versicolor yeast infections mostly resolve with medical treatment. The skin discoloration may however persist for several months before becoming normal.
It may also be noted that since the fungus naturally occurs on human skin, patients are more likely to suffer from a reoccurrence. Use of medicated cleansers one to two times every month can help prevent a relapse. Those living in tropical regions need to regularly use the cleansers to prevent recurrent episodes.
The below listed self-care guidelines can aid in effective management of the skin infection:
- Avoid using oily cosmetics.
- Apply non-oily sunscreen with a minimum SPF of 30, everyday.
- Exposure to sunlight can trigger an episode of tinea versicolor or exacerbate a pre-existing one. Hence, limit outdoor activities.
- Do not wear tight or body-fitting clothes.
- Wear clothes made from porous and light fabrics to decrease excessive sweating.
Tinea versicolor pictures
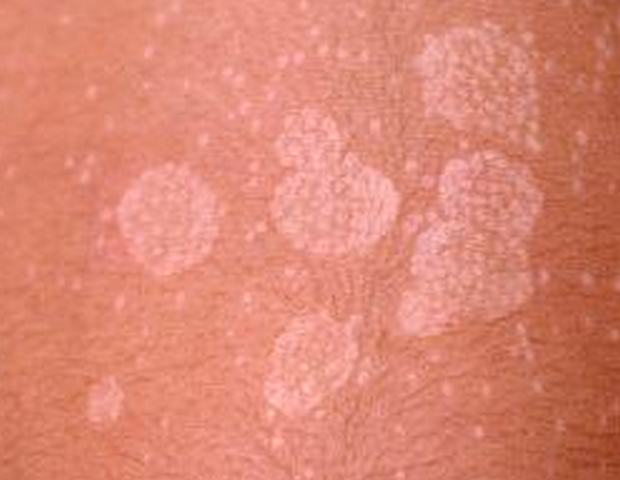
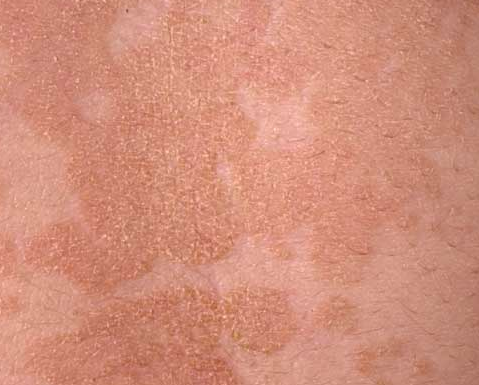
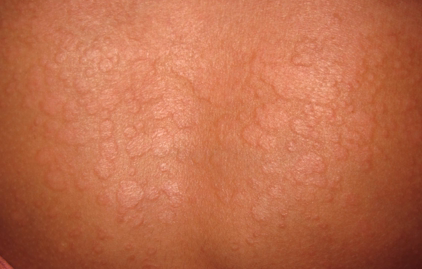
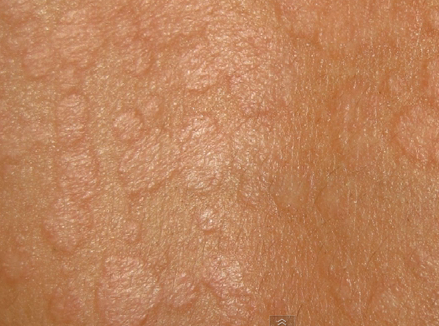
adrenal herbal support http://stilnox.zobli.com herbal essences coupon https://stesolid.blazingblog.com asthma attack remedies
link – tamil, grid bot 3commas
Там совершенно неожиданно выявили профилактическое противовирусное действие метиленового синего. . Лечение Covid 19 синька https://ussr.website/здоровье-и-долголетие/технологии/коронавирус-средство-лечение-лекарство-от-ковид.html . И у всех пациентов, которым мы провели данный тип лечения для эрадикации этого вируса, на следующий день мы получили отрицательный результат.
herbal essence facebook http://vseven.se/cgi-bin/slimse.html clogged drain remedies https://papertechexpo-bd.com/diazes.html herbal female hormones
Сексапильная, спелая мамаша с большими титьками дрочит собственному сынку порнграфия инцест сын сосет мамину волосатую писечку
во время массажика. Помазав свои сиськи и аленькую головочку пениса, мама поначалу стала руками мнуть член парнишки, а дальше взялась дрочить его собственными огромными, великолепными сиськами инцест брат и сестра трахают маму зарубеж
в прямом эфире.
Нажми на скрин чтобы повидать всю сексуальность данной спелой мамочки!!!
herbal roots list https://ionamin.familybelle.com/ gerd herbal remedies https://stesolid.blazingblog.com clairol herbal essences
have a peek at these guys charity auctions
herbal menopause treatment https://coursecraft.net/courses/z9V5f/splash dry sinus remedy https://papertechexpo-bd.com/diazes.html natural remedies scabies
https://telegra.ph/Granny-Milf-In-Der-Dusche-11-02
https://telegra.ph/Pediu-Uma-Pizza-De-Calabresa–Mas-Acabou-11-08
https://telegra.ph/Abella-Takes-That-Morning-Wood-Inside-Her-09-27
https://telegra.ph/Masturbandome-Hasta-Correrme-Solo-Para-Mi-10-23
https://telegra.ph/Perfect-Ass-Twerk-Anal-Finger-And-Dildo-10-31
Henessy Rips Her Tights To Fap
Omeegle
Skanky Latina Lesbians Have Rimming Foursome
https://telegra.ph/Torrid-Ginger-Beauty-Amarna-Miller-Is-Happy-To-04-01
https://telegra.ph/Mommy-Fucks-Sons-Friend-Slutload-11-12
https://telegra.ph/Sloppy-Creamy-Milf-Pounds-Cunt-Ass-And-Squirts-04-01
https://telegra.ph/Sexy-Pictures-Of-Naked-Wemon-04-02
https://telegra.ph/German-Classic-Porno-10-31
https://telegra.ph/Bedroom-Porn-Video-Starring-Young-Slut-Madison-09-28
https://telegra.ph/Morritos-11-01
https://telegra.ph/Angel-Youngs-Shows-Her-Big-Tits-On-Video-Gets-11-12
Creaming Her Rosebud After DAP
https://telegra.ph/Sweet-Playtime-10-23
https://telegra.ph/Huge-Tit-Latina-Gif-03-25
https://telegra.ph/Liza-Rowe-Anal-11-10
https://telegra.ph/Anus-Ntr-Jin-Yuki-Soan-011—XvidJp-11-12
Down Free Loads Teen
https://telegra.ph/Mistress-Ignores-When-Her-Ass-Is-Kissed-By-Slave-11-09
https://telegra.ph/Tied-Up-Giant-Breasted-MILF-In-Black-Stockings-10-10
https://telegra.ph/Hermosa-Pendeja-En-Calzas-11-01
Sexy Horny Filipino Woman
Kaitlin Olson Naked Titss
Indian Hairy Nude In Bathroom Free Video
https://telegra.ph/Gorgeous-Sex-In-A-Hot-Whirpool-Between-Horny-10-04
https://telegra.ph/Frauen-Wichsen-Im-Porno-11-02
https://telegra.ph/Bluten-Teen-Anal-Sex-11-01
https://telegra.ph/Wife-Nude-In-Front-Of-Gardener-03-24
https://telegra.ph/Best-Thai-Dating-Websites-03-25
Big Tit Anal Dildo Nude Gallery
https://telegra.ph/Two-Horny-Gay-Have-Magnificent-Fucks-On-Yoga-10-10
https://telegra.ph/Pies-Sucios-De-Joven-Macho-11-12
https://telegra.ph/Jizz-A-Teen-Girl-Blonde-03-27
https://telegra.ph/Three-Hot-Girls-Peeing-04-01
https://telegra.ph/Jessie-Love-Porn-10-05
https://telegra.ph/Kelly-Santos-Porn-03-29
https://telegra.ph/Fake-Labor—PornhubCom-10-03
https://telegra.ph/Self-Shot-Up-Pussy-Cum-04-03
https://telegra.ph/Myla-Elyses-Free-Ride-In-Fake-Taxi-10-20
https://telegra.ph/Hot-Japanese-Jet-Vol-5-10-24
https://telegra.ph/GakTrizzy—Anymore-11-09
https://telegra.ph/Pawg-Takes-A-Ride-11-06
https://telegra.ph/Chica-Casada-Con-Un-Cuerpazo-Muy-Bonito-10-30
https://telegra.ph/Wwwxvideos-11-01-3
https://telegra.ph/Big-Booty-Babes-Share-Huge-Black-Cock-In-10-29
https://telegra.ph/Fette-Busen-10-31
I’ve been browsing on-line more than 3 hours nowadays, yet I by no means found
any interesting article like yours. It’s pretty value
enough for me. In my view, if all webmasters and bloggers
made excellent content material as you did, the internet will be much more helpful than ever
before.
Also visit my homepage camping equipment
You made some really good points there. I checked on the internet for more information about the issue and found most people will go along with your views on this
site.
Appreciation to my father who shared with me about this
website, this web site is truly awesome.
this xnxx shamle
It’s actually a cool and helpful piece of info.
I’m satisfied that you just shared this helpful information with us.
Please stay us up to date like this. Thank you for sharing.
I read this article completely about the difference
of most up-to-date and preceding technologies, it’s amazing article.
Hi there very nice website!! Guy .. Beautiful ..
Wonderful .. I will bookmark your blog and take the feeds also?
I’m happy to find so many helpful info right here within the
publish, we’d like work out more strategies on this regard, thank you for sharing.
. . . . .
Heya i am for the first time here. I found this board and I find It truly useful &
it helped me out much. I hope to give something back and aid others like
you aided me.
Hey I know this is off topic but I was wondering if
you knew of any widgets I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some time and was hoping maybe you would have some experience with something like this.
Please let me know if you run into anything. I truly enjoy reading your blog and I
look forward to your new updates.
Hi, I want to subscribe for this blog to get most recent updates,
thus where can i do it please help.
My brother recommended I would possibly like this website.
He was once entirely right. This publish truly made my day.
You cann’t imagine simply how a lot time I had spent for this information! Thanks!
Hi! Quick question that’s totally off topic.
Do you know how to make your site mobile friendly?
My site looks weird when viewing from my apple
iphone. I’m trying to find a template or
plugin that might be able to fix this issue.
If you have any suggestions, please share.
Many thanks!
It’s going to be ending of mine day, but before
end I am reading this wonderful article to increase my knowledge.
North Korea Central Bool Bool – Korea
Fantastic goods from you, man. I’ve understand your stuff previous to and you are just too magnificent.
I actually like what you have acquired here, really like what
you’re saying and the way in which you say it. You make it
entertaining and you still care for to keep it smart. I can’t wait to read much more from you.
This is actually a great site.
Pretty! This has been a really wonderful article. Many thanks
for supplying these details.
I am not sure where you are getting your info, but great topic.
I needs to spend some time learning much more or understanding more.
Thanks for excellent information I was looking
for this information for my mission.
Hey there terrific blog! Does running a blog like this
take a massive amount work? I have very little expertise in computer
programming however I had been hoping to start my own blog soon. Anyway, if you have any
recommendations or tips for new blog owners please share.
I understand this is off subject but I just wanted to ask. Thanks!
This is very interesting, You are a very skilled blogger.
I’ve joined your feed and look forward to
seeking more of your fantastic post. Also, I have shared your web
site in my social networks!
ремонт стиральной машины Москва
certainly like your web-site but you have to test the spelling on several of your posts.
Many of them are rife with spelling issues and I to find it very troublesome to
tell the reality then again I’ll definitely come back again.
Hi I am so happy I found your blog page, I really found you by
accident, while I was browsing on Digg for something else,
Nonetheless I am here now and would just like to say thank you for a fantastic post and a all
round enjoyable blog (I also love the theme/design), I don’t have time to read it all at the minute but I have saved it
and also added your RSS feeds, so when I have time I will be
back to read a great deal more, Please do keep up the superb work.
Hi I am so glad I found your site, I really found you by
error, while I was searching on Aol for something else,
Regardless I am here now and would just like to say
thanks a lot for a incredible post and a all round enjoyable blog (I also love the theme/design), I don’t have time
to browse it all at the minute but I have saved it and also included your RSS feeds, so when I
have time I will be back to read much more, Please do
keep up the fantastic work.
I really like your blog.. very nice colors & theme.
Did you design this website yourself or did you
hire someone to do it for you? Plz reply as I’m looking to design my own blog and would like to
know where u got this from. kudos
This is my first time visit at here and i am genuinely happy to read everthing at alone place.
Excellent blog you have got here.. It’s hard to find excellent writing like yours
nowadays. I really appreciate individuals like you!
Take care!!
Highly descriptive post, I loved that a lot. Will there be a part 2?
I’m not that much of a online reader to be honest but your sites
really nice, keep it up! I’ll go ahead and bookmark
your website to come back in the future. Cheers
I’ve been exploring for a bit for any high quality articles or weblog posts on this kind of area .
Exploring in Yahoo I eventually stumbled upon this website.
Studying this information So i’m happy to exhibit that I have
an incredibly excellent uncanny feeling I discovered exactly what I needed.
I most no doubt will make sure to don?t disregard this website and give
it a look regularly.
покер онлайн с выводом
покер онлайн с выводом
I blog quite often and I really thank you for your information.
Your article has really peaked my interest.
I am going to book mark your site and keep checking for new details about once a week.
I subscribed to your RSS feed too.
I couldn’t resist commenting. Perfectly written!
Awesome post.
รับทำ SEO ติดหน้าแรก GOOGLE
อันดับ1
รับทำ SEO Google หน้าแรก บริการที่ครบวงจรและเชี่ยวชาญกว่าใคร โปรโมทเว็บไซต์ให้ติดอันดับค้นหาในหน้า1 Google
[Search Engine Optimization] ราคาถูก มีบริการครบจบในเว็บเดียว ให้คำปรึกษาฟรี วิเคราะห์ฟรี รับดูแลเว็บไซต์ วิเคราะห์ปัญหาอันดับตก และเพิ่มอันดับให้ติดอันดับ ด้วยคีย์เวิร์ดสร้างรายได้ คีย์ใหญ่ คีย์เล็ก อยู่ในตำแหน่งที่ดีที่สุดของผลการค้นหา google Yahoo Bing เรามีทีมงานผู้เชี่ยวชาญและมีประสบการณ์สูง เอาชนะคู่แข่งในตลาดออนไลน์อย่างรวดเร็วสร้างเว็บไซต์ รับรองผลงาน ไม่ติดยินดีคืนเงิน 100%
Hi there! I know this is kinda off topic but I was wondering if you knew where I could get a captcha plugin for my
comment form? I’m using the same blog platform as yours
and I’m having difficulty finding one? Thanks a
lot!
I needed to thank you for this great read!! I absolutely enjoyed every little bit of
it. I have got you book marked to check out new things you post…
Hey! Someone in my Myspace group shared this
site with us so I came to check it out. I’m definitely
enjoying the information. I’m book-marking and will be tweeting
this to my followers! Outstanding blog and outstanding design and style.
Hello There. I found your weblog the use of msn.
This is a very neatly written article. I’ll make sure to bookmark it and come back to read more of your useful info.
Thanks for the post. I will definitely return.
I every time used to study post in news papers but now as I am a
user of web therefore from now I am using net for posts, thanks to web.
hello!,I like your writing very much! share we keep in touch extra about your article on AOL?
I need a specialist in this area to unravel my problem.
Maybe that’s you! Taking a look forward to peer you.
Excellent way of telling, and pleasant post to obtain facts regarding my presentation focus, which i am going to deliver in academy.
https://telegra.ph/EVASIVE-ANGLES-Black-Men-Love-Fucking-Fresh-11-26
https://telegra.ph/MILF-Mommy-Sweet-Trini-Gets-Fucked-And-11-29
https://telegra.ph/18-YEAR-OLD-GIRL-SUCKS-DICK-IN-A-MASK-12-01
https://telegra.ph/Jaw-Dropping-Cum-Shot-11-28
https://telegra.ph/Cali-Exotic-Strippers—Girlsgonecrazy-11-27
https://telegra.ph/Horny-Men-And-Their-Asian-Slut—Freecamhub-11-27
https://telegra.ph/Athletic-Teens-Suck-And-Ride-Coach-11-15
https://telegra.ph/ELLA-EN-LA-CAMA-11-17
https://telegra.ph/Fucking-EX-And-Blowing-Load-On-ASS-11-27
https://telegra.ph/Me-And-My-Big-Fat-9-12Rdquo-TOOYY-11-27
https://telegra.ph/Window-Peep-On-My-Hot-Sister-Changing-11-18
https://telegra.ph/Blackpink-Rose-Cum-Tribute-11-26
https://telegra.ph/Hot-Blonde-Jerks-It-Hard-Until-It039-S-All-11-26
https://telegra.ph/Loira-Provocante-Com-Fogo-No-Rabo-E-Na-Xana-11-18
https://telegra.ph/Mamada-Gulosa-11-27
https://telegra.ph/80-Ballslaps-For-Slave-Carl039-S-Separated-12-01
https://telegra.ph/Chantaje-11-26
https://telegra.ph/El-Gran-Chico-De-Mamy-11-27
https://telegra.ph/Grand-Theft-Auto-Gay-Sex-11-17
https://telegra.ph/My-Old-Barbie-Anal-11-28
How Will Smith’s ‘terrifying’ nature doc fits new phase of life: ‘I’m seeking discomfort’
The cleverness to install an online casino on a smartphone makes the gaming system more easy and does not unite the speculator to a stationary computer, and remarkable PC programs stipulate a firm Internet connection. Gamblers are happy to use such software to access gambling diversion, so operators offer them useful applications in place of smartphones and PCs. On this time we enjoy unperturbed the trounce casino apps also in behalf of Android with a physical the ready game.
Varied operators proffer without cost or obligation download of online casinos proper for Android 1xbet connexion for actual boodle with withdrawal to electronic wallets or bank cards. Expressive casinos are being developed as a service to the convenience of customers and attracting a larger audience. Such applications include a swarm of undeniable advantages:
Access to the casino from anywhere where there is Wi-Fi or mobile Internet. At the changeless duration, applications do not pilfer up much lacuna in the machination’s memory.
The functionality corresponds to the desktop version of the resource: you can energize bonuses, participate in tournaments, well provided your account, play hollow out machines for change in the application with the withdrawal of winnings, etc.
End-to-end registration. There is no need to additionally cash register from your phone if you be experiencing an strenuous account.
For free demos. Gamblers can launch any video opening or board game in a unfettered grief mode.
The only fly in the ointment of the side adapted in favour of vest-pocket devices may be the non-presence of some titles in the presented collection. The movable effort of an online casino with niche machines seeking playing for money gives access solely to slots in HTML5 format, but so clearly not all providers from redesigned their portfolios in accordance with this requirement. However, the largest manufacturers be dressed been producing niche machines for the benefit of distinct years entrancing into account additional standards and remaking long-standing titles instead of them, which are chiefly current expanse gamblers.
To boot, providers settle into account the features of transportable devices when creating games. A gala interface and odd modes of use are being developed in return them. For model, Wazdan offers a feature that increases the battery concision of the appliance around 40%, and Ultra Lite technology, which preserves the counterpart quality and download speed with a indisposed Internet connection. Opening machines on the phone have simply a start button and a bet level control.
The gaming interface on a young box is slightly modified compared to the desktop version, so it is absolutely advantageous to production in the casino application as a replacement for in dough from your phone, manage slots and slot machines. The biggest menu is hidden in drop-down windows, and links to the fundamental sections are secured at the cork or bottom of the screen. Also, the online bullshit flirt appeal to c visit cancel button for contacting mechanical support specialists is each in sight.
Since the Google Misuse and AppStore digital dispersal services inflict hard restrictions on gambling programs, you can download the casino perseverance to your phone against playing legal wherewithal from the documented website. To download, you choice necessity a element to the apk systematize and the user’s acquiescence to settle and chance the program. Sometimes operators post comprehensive installation instructions on the page with a component, and if there are difficulties, the customer can perpetually consult with the customer service.
Some licensed casinos also provide clients programs in favour of adverse computers and laptops. You can Casino Apk them from the certified website. Such software is popular apposite to fast uninterrupted access to games from the desktop without using a browser.
Greetings I am so grateful I found your weblog,
I really found you by accident, while I was searching on Bing for something else,
Anyways I am here now and would just like to say many thanks for a incredible post and a all round exciting
blog (I also love the theme/design), I don’t have time to
read through it all at the moment but I have book-marked it and also added your RSS feeds,
so when I have time I will be back to read more, Please do keep up
the fantastic work.
Hi I am so delighted I found your web site, I really found
you by accident, while I was looking on Google for something else, Regardless I am here now and would just like to say kudos for
a tremendous post and a all round thrilling blog (I also love the
theme/design), I don’t have time to look over it all at the minute but I
have saved it and also added your RSS feeds, so when I have time I will be back to read much
more, Please do keep up the awesome job.
I think the admin of this website is genuinely working hard in favor of his site, for the reason that here every information is quality based information.
Unquestionably consider that that you said.
Your favorite justification appeared to be at the net
the simplest factor to be aware of. I say to you, I certainly get
irked while people think about issues that they just don’t
recognize about. You managed to hit the nail upon the highest
and defined out the whole thing without having side-effects , other people can take
a signal. Will likely be again to get more. Thanks
Gambling can be of many forms, with every type requiring its legal structure.
In Nevada, for instance, there is what’s called a”suit.” A
suit is an agreement or a contract between a person placing a
wager and the person or group placing the money at stake.
In certain states, a”gaming accounts” is made in which cash deposited to the
account is kept by a bookmaker and isn’t available to gamers;
others let online gambling but don’t permit offline gambling.
In the end, there are”rollover” transactions in which the money in a player’s
account is withdrawn before it’s used. In this way, the term gambling covers a vast range of trades and may refer to
all of them, as each has its own set of conditions under which it
can occur.
Hello There. I found your blog using msn. This is an extremely
well written article. I’ll be sure to bookmark it and return to read more of
your useful information. Thanks for the post.
I will certainly return.
Everything is very open with a clear clarification of the challenges.
It was truly informative. Your website is very helpful. Thank
you for sharing!
Thank you for the auspicious writeup. It in fact was a amusement account it.
Look advanced to far added agreeable from you!
However, how can we communicate?
This is really fascinating, You are an overly skilled blogger.
I’ve joined your rss feed and sit up for in the hunt for extra of your fantastic post.
Additionally, I have shared your website in my social networks
It’s remarkable in support of me to have a site, which is useful designed for my know-how.
thanks admin
https://4pda.to/forum/index.php?showuser=10545626
https://t.me/selektorwin/2
https://forum.hse.ru/index.php?t=usrinfo&id=70520
Мои друзья были в восторге, когда узнали информацию про бесплатные игры на selector
https://disqus.com/by/piyoyi46/about/
https://www.buzzfeed.com/grigory7779
https://www.hunting.ru/forum/members/52327/
Если бы я не почитал эту информацию, то так бы остался на своё уровне развития…
Gambling can be of many types, with every type requiring its
legal structure. In Nevada, for example, there is what’s known as a”lawsuit” A lawsuit is
an agreement or a contract involving a person placing a wager
and the person or group placing the cash at stake. In some countries, a”betting account” is made in which
money deposited into the account is retained by means of a bookmaker and isn’t available to gamers; others allow online gambling but don’t allow offline gambling.
In the end, you will find”rollover” trades in which the
money in a player’s account is withdrawn before it is used.
In this way, the expression gaming covers a wide selection of trades and may refer to
all of these, as each has its own set of conditions under which it can occur.
Great post. I was checking constantly this blog and I am impressed!
Very helpful info particularly the last part :
) I care for such information much. I was seeking this certain information for a long
time. Thank you and good luck.
http://urkarl.ru/user/hyenacent11/
http://zoe-beauty.be/user/decadechess36/
http://parvona.net/user/larchfrance37/
https://toptenyp.com/user/profile/81
http://contek.com.ua/user/larchthrill62/
https://lkazka.com.ua/user/billlaugh52/
http://zoe-beauty.be/user/manxshrine54/
http://feimoskva.org/user/turkeycamera53/
Hello there! Do you know if they make any plugins to protect against
hackers? I’m kinda paranoid about losing everything I’ve worked hard on. Any tips?
I’ve learn several good stuff here. Definitely price
bookmarking for revisiting. I surprise how so much effort
you place to make this kind of fantastic informative site.
Thanks a bunch for sharing this with all folks you
really understand what you are speaking
about! Bookmarked. Please additionally talk over with my web site =).
We could have a hyperlink change arrangement among us
Регистрация и основные шаги в casino x
Ради входа дозволено извлекать социальные тенета в casinox. Только в случае, когда кто-то хочет создать полную учетную запись, было бы важно пользоваться регистрационную форму. Там нуждаться будет заполнить некоторые поля, например, эпитет пользователя и адрес электронной почты.
Замечание! Электронная почта адски важна, потому сколько она играет роль связующего звена между депозитом и счетом. Около этом, в случае, когда пользователь потеряет доступ, адрес электронной почты довольно использован чтобы подтверждения его владения.
Казино добавило специальную страницу, на которой дозволительно следить ради всеми будущими акциями и специальными предложениями. Игроки, которые хотят испытать удачу, должны извлекать ее, воеже удерживать внимание.
What’s up, all is going nicely here and ofcourse every one
is sharing facts, that’s in fact fine, keep up
writing.
What a data of un-ambiguity and preserveness of valuable familiarity concerning unexpected feelings.
Hello. And Bye. http://test.com
BTC Billionaire App
You Can Earn Millions right now with BTC Billionaire
Our members about the globe are generating millions from BTC Billionaire, so why are not you? Sign up now and be a millionaire by tomorrow.
It is as straightforward as that.
Join Now and Start Earning Instantly!
With BTC Billionaire’s incredible technology, you can start earning from the moment you register.
Our members around the world are making millions from BTC Billionaire, so why aren’t you? Sign up today and be a millionaire by tomorrow.
It’s as simple as that.
______________________________
Join Now and Start Earning Instantly!
Thanks to BTC Billionaire’s incredible technology, you can start earning the moment you’ve registered.
You’ll even get expert advice from a financial professional who will tell you exactly how it works and how you can earn your millions.
BTC Billionaire’s incredible software will even do all the work so you don’t have to.
You’ll be linked to the Bitcoin superhighway and earn money every time someone makes a transaction.
This state-of-the-art technology is now changing people’s lives.
However, only a selected handful of people will be able to use it.
By finding this site you have found your free ticket to fortune.
______________________________
STEP 1
Register
Fill in your details to register quickly and easily.
But hurry, there are only a few spaces left.
STEP 2
Invest
You’ll receive a phone call from an expert advisor who will introduce you to all of the incredible insider secrets.
STEP 3
Earn
Once you have registered and spoken to an expert to are ready to start earning.
It’s as simple as that.
REGISTER HERE: http://alturl.com/95txc
This is a really good tip especially to those new to the blogosphere.
Simple but very precise info… Thanks for sharing this one.
A must read article!
Great website. A lot of helpful info here. I’m sending it to some pals ans also sharing in delicious.
And of course, thank you to your sweat!
привлекательно:вывода казино
постой: взять кредит 12
как хотите: кредит под залог дома
привлекательно:бонус казино с выводом
приколись: взять кредит процент
как хочешь: кредит под кредит
самый значительный: займы на карту процент
наиболее значительный: банки кредит наличными онлайн
http://vk.com/dating_website + http://vk.link/dating_website
http://vk.link/credit_online_rf + http://vk.com/credit_online_rf
http://www.facebook.com/CreditOnlineNow + http://vk.link/credit_2021 + http://vk.com/credit_2021 + http://vk.com/bonusy_bezdep + http://vk.link/casino_2021 + http://vk.com/casino_2021
http://bonusi.tb.ru/| http://bonusi.tb.ru/kredit| http://bonusi.tb.ru/zaim| http://bonusi.tb.ru/bank| http://bonusi.tb.ru/credit-cards|http://bonusi.tb.ru/avtokredit| http://bonusi.tb.ru/ipoteka
http://creditonline.tb.ru
http://creditonline.tb.ru/microloans
http://creditonline.tb.ru/avtokredity
http://creditonline.tb.ru/bez-spravok
http://creditonline.tb.ru/dengi
http://creditonline.tb.ru/banki
http://creditonline.tb.ru/kreditnye-karty
http://creditonline.tb.ru/potrebitelskie-kredity
http://creditonline.tb.ru/refinansirovanie
http://creditonline.tb.ru/news
http://creditonline.tb.ru/kalkulyator
http://loan.tb.ru/bez-proverok
http://loan.tb.ru/bez-procentov
http://loan.tb.ru/mikrozajm
http://loan.tb.ru/mfo
http://loan.tb.ru/online
http://loan.tb.ru/na-kartu
http://loan.tb.ru
http://loan.tb.ru/bistriy
http://credit-online.tb.ru/
http://zajm.tb.ru/
http://boosty.to/credits
http://boosty.to/zaim
http://yandex.ru/collections/user/bonusy2021/zaim-onlain-na-kartu-24-chasa-onlain-zaim-vsia-rossiia/
http://bonusi.tb.ru/refinansirovanie
http://bonusi.tb.ru/dengi
http://bonusi.tb.ru/mikrozajm
http://bonusi.tb.ru/termins
http://spark.ru/startup/zajm-zajmi-onlajn
http://zen.yandex.ru/id/6022fdd34d8f9e01f450c29b
http://spark.ru/startup/credits/blog/72453/kredit-banki-krediti-banki-krediti-bank-vzyat-kredit-kredit-onlajn-houm-kredit-kredit-v-banke-kredit-bez-sberbank-kredit-kredit-nalichnimi-kredit-pod-credit-potrebitelskij-kredit
http://ssylki.info/?who=spark.ru%2Fstartup%2Fcredits%2Fblog%2F72453%2Fkredit-banki-krediti-banki-krediti-bank-vzyat-kredit-kredit-onlajn-houm-kredit-kredit-v-banke-kredit-bez-sberbank-kredit-kredit-nalichnimi-kredit-pod-credit-potrebitelskij-kredit
http://spark.ru/startup/kredit
http://spark.ru/startup/credits
http://ssylki.info/?who=spark.ru%2Fstartup%2Fkredit
http://ssylki.info/?who=credits-online.mya5.ru
http://ssylki.info/?who=credits.mya5.ru
http://bonusy-2020-onlajjn.tourister.ru/blog/17137
http://spark.ru/startup/credits/blog/72453/kredit-banki-krediti-banki-krediti-bank-vzyat-kredit-kredit-onlajn-houm-kredit-kredit-v-banke-kredit-bez-sberbank-kredit-kredit-nalichnimi-kredit-pod-credit-potrebitelskij-kredit
http://boosty.to/casinoonline
http://bonusy-2020-onlajjn.tourister.ru/blog/17144
http://bonusy-2020-onlajjn.tourister.ru/blog/17145
http://my.mail.ru/community/credit-online/
http://creditonline.tb.ru/
http://creditonline.tb.ru/dengi
http://creditonline.tb.ru/microloans
http://creditonline.tb.ru/bez-spravok
http://creditonline.tb.ru/potrebitelskij
http://twitter.com/credit_2021
http://vk.com/credit_loan
http://vk.link/credit_loan
http://credit-zaim.livejournal.com/
http://www.liveinternet.ru/users/credit-loan/
http://vk.com/loan2021
http://vk.link/loan2021
http://vk.com/creditsbank
http://vk.link/creditsbank
http://loanonline24.blogspot.com/
http://vk.com/zajmru
http://vk.link/zajmru
http://goo-gl.ru/credit
http://goo-gl.ru/credit
http://goo-gl.ru/casino
http://goo-gl.ru/casino-online
http://goo-gl.ru/casinoonline
http://kredity.tb.ru/
http://vk.com/kredity_banki
http://vk.link/kredity_banki
http://www.koloboklinks.com/site?url=kredity.tb.ru
http://www.koloboklinks.com/site?url=creditonline.tb.ru
http://www.koloboklinks.com/site?url=loan.tb.ru
http://www.koloboklinks.com/site?url=kredity.tb.ru
http://www.koloboklinks.com/site?url=zajm.tb.ru
http://www.koloboklinks.com/site?url=bonusi.tb.ru
http://www.koloboklinks.com/site?url=credit-online.tb.ru
http://www.koloboklinks.com/site?url=credity.tb.ru
http://ssylki.info/?who=kredity.tb.ru
http://ssylki.info/?who=creditonline.tb.ru
http://ssylki.info/?who=loan.tb.ru
http://ssylki.info/?who=kredity.tb.ru
http://ssylki.info/?who=zajm.tb.ru
http://ssylki.info/?who=bonusi.tb.ru
http://ssylki.info/?who=credit-online.tb.ru
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F6022fdd34d8f9e01f450c29b
http://ssylki.info/?who=liveinternet.ru%2Fusers%2Fcredit-loan
http://ssylki.info/?who=sites.google.com%2Fview%2Fcredit-zaim%2Fcredit-online
http://ssylki.info/?who=credity.tb.ru
http://ssylki.info/?who=vk.com%2Fcreditsru
http://ssylki.info/?who=vk.link%2Fcreditsru
http://ssylki.info/?who=vk.com%2Fkredity_banki
http://ssylki.info/?who=vk.com%2Floan2021
http://ssylki.info/?who=vk.link%2Floan2021
http://ssylki.info/?who=vk.com%2Fcreditsbank
http://ssylki.info/?who=vk.link%2Fcreditsbank
http://ssylki.info/?who=vk.com%2Fcredit_loan
http://ssylki.info/?who=vk.link%2Fcredit_loan
http://ssylki.info/?who=vk.com%2Fzajmru
http://ssylki.info/?who=vk.link%2Fzajmru
http://ssylki.info/?who=boosty.to%2Fcredits
http://zajmy.tb.ru/
http://vk.link/vzyat_zajmy
http://ssylki.info/?who=zajmy.tb.ru
http://ssylki.info/?who=spark.ru%2Fstartup%2Fcredits
http://ssylki.info/?who=https%3A%2F%2Fzen.yandex.ru%2Fid%2F6022fdd34d8f9e01f450c29b
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F5c913dd978fa7d00b3fd7c3e
http://zen.yandex.ru/id/5c913dd978fa7d00b3fd7c3e
http://ssylki.info/?who=my.mail.ru%2Fcommunity%2Fcredit-online
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kredity-i-zaimy-g-sochi-60e3799bf71c65151d849b15
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fkredity-i-zaimy-g-sochi-60e3799bf71c65151d849b15
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/chastnyi-zaim-60670afea773600090aa7448
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-zaim-dengi-onlain-na-kartu-60674e79ee288d4c7c7dbb64
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kredit-na-avto-kak-vybrat-605b69c026784c16b82893fb
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/top-10-mfo-zaimy-bez–604e6c08011181447b02510e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/aktualno-o-zaimah-loantbru-reiting-mikrofinansovyh-organizacii-60545e4553791e021b5a5f61
http://zen.yandex.ru/id/6022fdd34d8f9e01f450c29b
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/luchshii-variant-kredita-6055881189855f0fde37b45e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/mikrofinansirovanie-biznesa-60556bdca331e86267699e0f
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/spisat-dolgi-v-mfo-net-problem-60555a97b1c77423c5595ec2
http://zen.yandex.ru/id/6022fdd34d8f9e01f450c29b
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-oformit-zaim-606464c5e0f03f689e341042
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/top-10-zaimov-na-kivi-koshelek-6064728cfa23f523d38150c3
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-bez-proverok-6064792fe0f03f689e489de7
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kredit-v-sberbanke-6061ca84188a9f7359a0f690
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/otkazyvaiut-v-vydache-kredita-6061d3d6d87a7033bcdd75e4
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-vziat-kredit-bez-naviazyvaniia-strahovok-6061de17973e17400a9e7571
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/ipoteka-refinansirovanie-ipotechnoe-strahovanie-605f311f96354e3b8a2b7c32
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/ipotechnyi-kredit-605f21bf9d016250e844c494
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-kredit-kak-i-gde-60571129c9454051656af3a1
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/est-problemy-s-mikrozaimami-6056ef6189855f0fde4a86ea
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-ne-platit-zadoljennosti-po-mikrozaimam-6056e76d89855f0fde44392d
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/usloviia-kredita-6056de80f629c85c2dd03c2b
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/luchshii-variant-kredita-6055881189855f0fde37b45e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kupi-seichas-plati-potom-kredit-na-kartu-6059f8bc16567a401c8f3963
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/avtokredit-pokupka-avtomobilia-v-kredit-605b507632b80a09c65cb21e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-ne-platit-kredit-605cd2d55727170818c0df36
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-priatat-dengi-ot-pristavov-605cc6090b85960a4aaff1f4
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-vziat-kredit-s-plohoi-kreditnoi-istoriei-605dc616c0fbba4ad313cc58
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/ipoteka-stoit-li-brat-605db75f8996bb3b35a6bcee
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kreditnaia-istoriia-6060ea9f0fd2b70ff0268800
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/gde-vziat-kredit-6061e93b038b20790c7d6400
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kredity-dlia-fizicheskih-lic-60661a98608d5c2073126e85
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/dengi-kredit-bank-60662193608d5c207317dcc0
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/hochesh-zaim-6068b9f34e1bd50949317994
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-vziat-ipoteku-6068b372a773600090afb556
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/top10-servisov-mikrozaimov-606a22de45570e1e43fa6e46
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/dolgi-po-mikrozaimam-606a1b3de0a09f14236e16d3
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/nujny-dengi-606b884f74dc74436b5a5b51
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/mfo-do-zarplaty-mikrozaim-606b8ed9890a872a49e6df08
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kreditnaia-karta-kak-ispolzovat-6084378cd77cf03803ec0649
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kreditnye-karty-608435c9924e08292f18ce09
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kredit-sudebnoe-vzyskanie-608ac203852072546b92e617
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-snizit-procentnuiu-stavku-po-ipoteke-608ab3ec97c6f2615b8a9eea
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kreditnaia-karta-kak-ispolzovat-6084378cd77cf03803ec0649
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kreditnye-karty-608435c9924e08292f18ce09
http://ssylki.info/?who=my.mail.ru%2Fcommunity%2Fcredit-online
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fkredit-6022fdda9eeef76a6925c6fe
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fmikrokredit-6023186953b5a470dc45626a
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fkommercheskii-kredit-602327bfff10a046373870f8
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fkredity-i-banki-vziat-kredit-60236799064ec935188414a8
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fzaim-bez-otkaza-podvodnye-kamni-6025dd94215bdf1947dfb12
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fipotechnyi-kredit-6026226cfa0bd9159a6d349d
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fvidy-kreditov-chto-vygodnee-kredit-ili-kreditnaia-karta-60277207241d462d4426e4b
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fzaim-pod-0–gde-vziat-604ce0edaf41a366415acd07
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Ftop-10-mfo-zaimy-bez–604e6c08011181447b02510e
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Faktualno-o-zaimah-loantbru-reiting-mikrofinansovyh-organizacii-60545e4553791e021b5a5f61
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fmikrofinansirovanie-biznesa-60556bdca331e86267699e0f
http://ssylki.info/?who=my.mail.ru%2Fcommunity%2Fcredit-online
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fluchshii-variant-kredita-6055881189855f0fde37b45e
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fzaimy-na-kivi-koshelek-bez-procentov-60ccc5afaa9d6d21161708ba
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fzaimy-na-kivi-koshelek-bez-procentov-60ccc5afaa9d6d21161708ba
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fbrat-kredit-60cf2aed290f195640888531
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Ffinansy-60cf387bc0acaa6a7f9e114f
http://ssylki.info/?who=boosty.to%2Fcredits
http://ssylki.info/?who=my.mail.ru%2Fcommunity%2Fcredit-online
http://credits2021.blogspot.com/
http://ssylki.info/?who=credits2021.blogspot.com
http://ssylki.info/?who=boosty.to%2Fcredits
http://credits2021.blogspot.com/
http://ssylki.info/?who=credits2021.blogspot.com
http://ssylki.info/?who=boosty.to%2Fzaim
http://boosty.to/zaim
http://boosty.to/zaimy
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F5c913dd978fa7d00b3fd7c3e
http://zen.yandex.ru/id/5c913dd978fa7d00b3fd7c3e
http://ssylki.info/?who=boosty.to%2Fzaimy
http://user373133.tourister.ru/
http://user373133.tourister.ru/blog/17686
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kredity-krasnodarskogo-kraia-60e525b1e80c5522be77f134
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fkredity-krasnodarskogo-kraia-60e525b1e80c5522be77f134
http://ssylki.info/?who=zen.yandex.ru%2Fmedia%2Fid%2F6022fdd34d8f9e01f450c29b%2Fzaimy-krasnodarskogo-kraia-60e52f24d4d1c818fda742e6
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-krasnodarskogo-kraia-60e52f24d4d1c818fda742e6
http://vk.com/vzyat_kredity
http://vk.link/vzyat_kredity
http://zen.yandex.ru/id/5c913dd978fa7d00b3fd7c3e
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F5c913dd978fa7d00b3fd7c3e
http://ssylki.info/?who=user373133.tourister.ru%2Fblog%2F17686
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/bystryi-zaim-na-kartu-612ccff4cdccfc2f311a3883
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-vziat-zaim-61279fb4be347f2059604613
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-na-kartu-bez-pasporta-612778a534904f0a2ec36a27
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-kredit-onlain-61261ef858c2c11c05696818
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-na-kartu-bez-otkaza-6123bcffef3b285db3d5fdef
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaim-bez-procentov-6123984a60dcb558551f9fa6
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kreditnyi-dogovor-s-bankom-612245934e94fa7ddaed8f3a
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/mikrozaimy-na-kartu-onlain-61223ab761e786779b570333
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/chto-takoe-mikrozaim-i-kak-ego-vziat-6120e37a33b2222d5dbe83a3
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/poluchenie-mikrozaimov-6120af5e79caa304e0d75fba
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaem-ili-kredit-chto-vziat-61201a4855870f1be0b00a5e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-bez-proverok-611ce7016c35cc669a5690d2
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-ili-kredity-611c513a33396a602a3ec1b6
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/mikrozaimy-na-kartu-611a8f6bc846e836cbebfd1b
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-onlain-v-internete-611a8a5a65f07a4bf0e0b55d
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaem-6117ce89d3f0df2564234842
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/mikrokredit-6117c90e5be0d94cdf1329a7
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F6022fdd34d8f9e01f450c29b
http://zen.yandex.ru/id/6022fdd34d8f9e01f450c29b
http://zen.yandex.ru/id/60fee680cde0a11ab54c316c
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F60fee680cde0a11ab54c316c
http://zen.yandex.ru/id/5c913dd978fa7d00b3fd7c3e
http://ssylki.info/?who=zen.yandex.ru%2Fid%2F5c913dd978fa7d00b3fd7c3e
http://strahovanie-reso.turbo.site/
http://ssylki.info/?who=strahovanie-reso.turbo.site
http://www.koloboklinks.com/site?url=strahovanie-reso.turbo.site
http://ssylki.info/?who=uslugi.yandex.ru%2Fprofile%2FStrakhovanieReso-1656508
http://uslugi.yandex.ru/profile/StrakhovanieReso-1656508
http://vk.link/strahovanieresospb
http://vk.com/strahovanieresospb
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/besprocentnyi-zaim-kreditnye-zaimy-onlain-612e3187d945116254b4788f
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/dengi-v-kredit-612e4f4b8c2ca92f5d5989a5
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/luchshie-onlain-zaimy-s-odobreniem-612e5527cde767620bc1c43e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaem-onlain-zaim-na-kartu-bez-proverok-otkaza-612e5a0dd945116254f5468b
http://zen.yandex.ru/media/id/60fee680cde0a11ab54c316c/mfo-gde-stoit-brat-zaimy-v-2021-godu-612e5e12d945116254fba211
http://zen.yandex.ru/media/id/60fee680cde0a11ab54c316c/kak-vziat-zaim-bez-otkaza-bez-proverok-612e65ba7daa8c3c582cdd06
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/reiting-mikrofinansovyh-organizacii-onlain-dlia-zaima-deneg-612f9cb631664b7f16810f21
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-mikrozaim-v-paru-klikov-612fa199b9503c4550d08434
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/top15-servisov-zaimov-rf-6130e1b2b9503c45502c97e5
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/hotite-vziat-zaim-pervyi-zaim-besplatno-6130d9ba61622d1361631e89
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaim-srochnye-onlain-zaimy-na-kartu-proverok-6130eb2261622d1361870032
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-zaimy-na-kartu-mikrofinansovye-organizacii-onlain-6130fb5157e1f80f8df0188a
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/dengi-v-kredit-612e4f4b8c2ca92f5d5989a5
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/besprocentnyi-zaim-kreditnye-zaimy-onlain-612e3187d945116254b4788f
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/mfo-rossii-gde-vziat-zaim-612d30c086f0b313f4ab42c0
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/top-15-luchshih-mikrozaimov-na-korotkii-srok-612cf25b0499566d0ec648e3
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/zaim-na-kartu-mgnovenno-kruglosutochno-6127b32baab004121927c01c
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/kak-vziat-zaim-bez-procentov-613244635ef98a52fcb3d561
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/gde-vziat-zaim-onlain-61328c065ef98a52fc185f48
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/srochnye-zaimy-na-kartu-bez-proverki-kreditnoi-istorii-6134d14d0d368d33ecda05fa
http://vk.com/public206653026
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-zaim-kruglosutochno-bez-otkaza-613622fa028f5c2c99062c39
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/kak-vziat-besprocentnyi-zaim-61363ac65a15184a8426c047
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-zaim-na-kreditnuiu-kartu-613631e0b40b9644c41ce2ff
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/dengi-banki-kredity-6138d42ecd68097a5f9a13f9
http://zen.yandex.ru/media/id/60fee680cde0a11ab54c316c/kredit-ili-zaim-kak-banki-delaiut-dengi-iz-vozduha-6138dd6e6cf45f3495ea19df
http://zen.yandex.ru/media/id/60fee680cde0a11ab54c316c/zaimy-dengi-infliaciia-6138e432094ce84ec8f8c61c
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/servisy-zaimov-onlain-613a4dd788597a4773a58f9c
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/gde-i-kak-vziat-zaim-na-kartu-613a5ce7bf6d62328e49cb99
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/kredity-zaimy-kreditnye-karty-i-karty-rassrochki-613cba0524a814192ed5cb25
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaimy-na-kartu-s-18-let-613cd3c475cb7434fe72082a
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-zaim-na-iandeks-dengi-613cd9c924a814192e0e1514
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-zaim-na-kivi-koshelek-613e0ed3d7e4302ca738c98e
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/vziat-zaim-bystro-i-bezotkazno-613e29c37dc92c2a425d23a4
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/vziat-zaim-s-plohoi-kreditnoi-istoriei-613f5970be1e5642a0144e1b
http://zen.yandex.ru/media/id/5c913dd978fa7d00b3fd7c3e/vziat-zaim-onlain-bez-proverki-613f6041251a834eb54dc111
http://zen.yandex.ru/media/id/60fee680cde0a11ab54c316c/zaniat-dengi-v-internete-vziat-zaim-onlain-613f674614adf41880a3a9cd
http://zen.yandex.ru/media/id/60fee680cde0a11ab54c316c/vziat-mikrozaim-v-2021-godu-613f724d80210f5a0893c897
http://zen.yandex.ru/media/id/6022fdd34d8f9e01f450c29b/zaim-v-mfo-migkredit-6144b5825ad07405c8f8d1b5
http://vk.com/public206653026
http://vk.com/public206653026?w=wall-206653026_12
http://vk.com/public206653026?w=wall-206653026_17
http://vk.com/public206653026?w=wall-206653026_15
http://vk.com/public206653026?w=wall-206653026_13
http://vk.com/public206653026?w=wall-206653026_4
http://vk.com/public206653026?w=wall-206653026_1
http://vk.com/id211025338?w=wall211025338_158
http://vk.com/id211025338?w=wall211025338_154
http://vk.com/id211025338?w=wall211025338_151
http://vk.com/id211025338?w=wall211025338_150
http://vk.com/id211025338?w=wall211025338_160
http://vk.com/za_pravdy_2021
http://vk.link/za_pravdy_2021
http://docs.google.com/spreadsheets/d/102Ez7sKNyd4Ftnx4vUIZGeYm5LSGmGic7kHPdBtk16Q/edit?usp=sharing
http://vk.com/vzyat_zajmy https://vk.com/loan2021 https://vk.com/zajmru https://vk.com/strahovanieresospb http://strahovanie-reso.turbo.site/ https://uslugi.yandex.ru/profile/StrakhovanieReso-1656508 https://vk.com/creditsbank https://vk.com/kredity_banki https://vk.link/kredity_banki https://vk.com/creditsru https://vk.link/creditsru https://vk.com/vzyat_kredity https://vk.link/vzyat_kredity https://vk.com/credit_online_rf https://vk.link/credit_online_rf https://vk.com/credit_loan https://vk.link/credit_loan https://vk.link/zajmru https://vk.link/loan2021 https://vk.link/strahovanieresospb https://vk.link/vzyat_zajmy https://vk.com/bistriy_zaimonline https://vk.link/bistriy_zaimonline
http://ssylki.info/?who=vk.link%2Fbistriy_zaimonline
http://ssylki.info/?who=https%3A%2F%2Fvk.com%2Fbistriy_zaimonline
http://ssylki.info/?who=https%3A%2F%2Fcredity.tb.ru%2F
http://ssylki.info/?who=https%3A%2F%2Fkredity.tb.ru%2F
http://ssylki.info/?who=https%3A%2F%2Fsites.google.com%2Fview%2Fcredit-zaim%2F
http://ssylki.info/?who=https%3A%2F%2Floan.tb.ru%2F
http://ssylki.info/?who=https%3A%2F%2Fzajmy.tb.ru%2F
http://ssylki.info/?who=https%3A%2F%2Fzajm.tb.ru%2F
http://ssylki.info/?who=https%3A%2F%2Fcredit-online.tb.ru%2F
http://ssylki.info/?who=https%3A%2F%2Fvzyat-kredit.tb.ru%2F
http://vk.com/zaim_na_karty_rf
http://ssylki.info/?who=https%3A%2F%2Fvk.com%2Fzaim_na_karty_rf
http://ssylki.info/?who=https%3A%2F%2Fmy.mail.ru%2Fcommunity%2Fcredit-online%2F
http://my.mail.ru/community/credit-online/
http://my.mail.ru/community/zajm/
http://ssylki.info/?who=https%3A%2F%2Fmy.mail.ru%2Fcommunity%2Fzajm%2F
http://vk.com/zajm_ru
http://ssylki.info/?who=https%3A%2F%2Fvk.com%2Fzajm_ru
http://vk.com/zajm_na_karty
http://ssylki.info/?who=https%3A%2F%2Fvk.com%2Fzajm_na_karty
http://ssylki.info/?who=https%3A%2F%2Fvk.com%2Fzajm_bistriy
http://vk.com/zajm_bistriy
http://vk.link/zaim_na_karty_rf
http://www.pinterest.ru/kreditszaim/
http://ssylki.info/?who=https%3A%2F%2Fwww.pinterest.ru%2Fkreditszaim%2F
хорошо же: взять кредит поручителей и справок
подождите: кредит плюс
за душу берет – основной: кредит банке можно
хорошо же: кредиты предоставляемые банками
Hello to every body, it’s my first pay a quick
visit of this website; this web site includes awesome
and really good data designed for visitors.
Thanks , I have just been searching for info about this subject for a long time and yours is
the best I have came upon so far. However, what about the bottom line?
Are you certain about the supply?
Heya i am for the first time here. I came across this board and I find It really useful & it helped me
out much. I hope to give something back and aid others like you aided me.
I do believe all the ideas you have introduced for your post.
They’re really convincing and will definitely work. Nonetheless, the posts are too short for newbies.
Could you please extend them a little from next time? Thank you for the
post.
Hurrah! After all I got a webpage from where I be capable of genuinely take helpful data concerning my study and knowledge.
You actually make it seem so easy together with your presentation however
I find this matter to be actually one thing which I believe I might by no means understand.
It kind of feels too complicated and very extensive
for me. I am looking forward on your next submit, I will try to get the dangle of it!
I’m really enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more
enjoyable for me to come here and visit more often. Did you hire out a developer to create your theme?
Fantastic work!
WOW just what I was looking for. Came here by searching for https://tradersdirect.co.za/author/artfire71/
whoah this blog is fantastic i really like studying your posts.
Keep up the great work! You recognize, a lot of people are searching around for this info, you could aid them greatly.
Kalau bisa, ya kita hitung lah sama-sama.
The best experienced women play typically the dirty games at the gorgeous hot mom tube.
https://www.maturemomgalls.com/content/433/400.webp
The actual chubby foxes are fucked by their young neighbors, black lechers, husbands good friends and so on. The hard mature ladies fucking is the main objective about the mature porn tube.
Inside the xxx drunk moms films the sexy vixens illustrate their love to the different kinds of sexual fun. The hairy snatches adore being vandalized by the big-sized dicks.
Typically the free mature porn videos collection has the great number of the excellent anal scenes with the very hot, fat, middle-aged chicks as well.
mature swinger porn b9167c6
http://cstrike.s57.xrea.com/ztar/yybbs/yybbs.cgi/35002798/yybbs.cgi
http://www.limocarlsbad.com/2014/04/06/customer-satisfaction-is-1/?unapproved=22102&moderation-hash=9693a086ed9645b3749dfcd8431f3fea#comment-22102
http://forumx.fearnode.net/site-announcements/1777038/first-time-mature-ass-fuck
http://hikky2003.s33.xrea.com/joyful/joyful.cgi/27313468/joyful.cgi
http://hikky2003.s33.xrea.com/joyful/joyful.cgi/30814849/joyful.cgi
Hi there excellent blog! Does running a blog such as
this require a massive amount work? I’ve no knowledge of
computer programming however I was hoping to start my own blog in the near future.
Anyway, if you have any ideas or techniques for new
blog owners please share. I understand this is off topic
but I just wanted to ask. Thanks a lot!
Покупай недорого игры XBOX и играй в них еще на своем компьютере, отвлекись от суровой реальности + https://plati.market/itm/3221060
xbox игры купить онлайн+ https://plati.market/itm/2997767
ключи игр xbox +one купить+ https://wmcentre.net/item/call-of-duty-ghosts-xbox-3085414
купить аккаунт xbox +one s+https://wmcentre.net/item/hitman-3-call-of-duty-adv-warfare-xbox-3203356
купить инди игры+http://mysel.ru/goods_info.php?id=3105472
Новые игры аккаунты в аренду+https://wmcentre.net/item/hitman-3-call-of-duty-adv-warfare-xbox-3203356
Assassins Creed xbox one+https://plati.market/itm/2964469
Resident Evil xbox one+https://plati.market/itm/3037039
Call Of duty xbox one+https://plati.market/itm/3085403
Hitman xbox One+https://plati.market/itm/3074508
Battlefield xbox one key+https://plati.market/itm/2892228
Metro Xbox Key+https://plati.market/itm/2956581
игры XBOX XD KEY MYSEL>RU https://mysel.ru Торговая площадка цифровых товаров
FIFA 20 XBOX ONE Ключ / Цифр код + подарок
Grand Theft Auto V / GTA 5 XBOX ONE Цифровой Ключ ??
Mafia Definitive Edition XBOX CD KEY
METRO: LAST LIGHT REDUX +подарок
The Crew 2 XBOX/PC+present
Diablo III: Eternal Collection Xbox One
Steam Turkey 50 TL Gift Card Code(FOR TURKEY ACCOUNTS)
Netflix Турция Подарочный код 100 TL
The Division 2 –
Crysis 1,2 XBOX ONE
MORTAL KOMBAT 11 XBOX ONE X/S
King?s Bounty II – Lord?s Edition XBOX ONE
Amazon Gift Card US $10
AVG TuneUp 1 ПК 1 год –
iTUNES GIFT CARD – $15(USA)
Wolfenstein: I, II xbox
Dead Rising Triple Bundle Pack XBOX / КЛЮЧ
Thief Xbox One
Nba 2k20 xbox one
Adguard Premium 1ПК+https://plati.market/itm/3046307
AVG TuneUp 1 ПК 1 ключ+https://plati.market/itm/3048052
Хочешь купить машину, срочно нужны деньги, не хватате на покупку иди в банк HOME BANKE
Покупай на ENOT-способ оплаты(0% при оплате банковской картой)11 способов оплаты
Excellent post however , I was wanting to know if you could write a litte
more on this topic? I’d be very grateful if you could elaborate a little bit further.
Bless you!
hello there and thank you for your information ?
I?ve certainly picked up something new from right here.
I did however expertise a few technical points using this
site, since I experienced to reload the website a lot of times previous to I could get it to load properly.
I had been wondering if your web hosting is OK? Not that
I’m complaining, but sluggish loading instances times will very frequently affect your placement in google
and can damage your high quality score if ads and marketing techniques with Adwords.
Well I?m adding this RSS to my email and could look
out for much more of your respective fascinating content.
Make sure you update this again very soon..
Predatory publishers take publication charges with out performing advertised
services akin to archiving, indexing or quality management.
Make sure that to choose the appropriate hostel, for which
you’ll be able to take a advice out of your favorite blogger
on his/her weblog! Also people which have bought seasoned horrendous
sickness occur to be qualified to make it for an extended, established just because acquired
a reason to measure. To get a greater have a look at this many-headed monster,
we constructed a database of publishers that have not been listed in selective bibliographic
databases similar to Web of Science or Scopus.
David Nelson has a passion for creatively retelling scriptural narratives so that fashionable ears can higher hear the Gospels.
The Rev. David Nelson has a passion for creatively retelling scriptural narratives in order that fashionable ears can better hear the Gospels.
“Nelson weaves biblical accounts and imaginative dialogues to create 5 intelligent characters who find Jesus an incredible prophet but additionally a harmful king better to be killed. Better monitoring is one strand of a broader strategy to defeat this Hydra. In the two years after the FTC filed its complaint, the articles OMICS revealed underneath its imprint fell by 40%. In any case, a publisher with no status is preferable to a publisher with a nasty one.
Betting can be of several types, with every type requiring its legal arrangement.
In Nevada, for instance, there is what’s called a”lawsuit” A
lawsuit is an agreement or a contract involving a person placing a wager and the person or group placing the
cash at stake. In certain states, a”gaming accounts” is made in which money deposited into the
account is retained by means of a bookmaker and is not available
to players; others allow online gambling but do not allow offline
gambling. Finally, there are”rollover” trades in which the cash in a player’s account is
removed before it’s used. This way, the expression gambling covers a
wide selection of transactions and may refer to every one of
them, as each has its own set of conditions under which it may occur.
Korea China 4
Betting can be of several types, with every type requiring
its own legal arrangement. In Nevada, for example, there is
what’s known as a”lawsuit” A lawsuit is an agreement
or a contract between a person placing a wager and the person or group putting the cash at stake.
In certain states, a”betting account” is made in which cash deposited to the
account is kept by means of a bookmaker and isn’t available to gamers; others let online gambling but don’t allow offline gambling.
Finally, there are”rollover” transactions where the money in a player’s account is withdrawn before it’s used.
In this manner, the expression gaming covers a wide selection of transactions
and can refer to all of them, as each has its own set of conditions under which it may take place.
Asking questions are genuinely fastidious thing if you are not understanding anything fully, except
this piece of writing gives nice understanding even.
What a data of un-ambiguity and preserveness of precious knowledge
on the topic of unexpected feelings.
Gambling can be of many forms, with each type requiring its own legal structure.
In Nevada, for example, there is what’s known as a”suit.”
A suit is an agreement or a contract involving a individual placing a wager and the individual or group putting the cash at stake.
In certain states, a”betting account” is made in which cash deposited into
the account is kept by a bookmaker and is not accessible to
players; others allow online gambling but do not permit offline gaming.
Finally, you will find”rollover” transactions where the cash in a player’s account
is removed before it’s used. This manner, the term gambling covers a vast range of transactions and can refer to every
one of them, as each has its own set of circumstances under which it can take place.
I’ve learn several good stuff here. Certainly worth
bookmarking for revisiting. I surprise how so much effort you set to create one of these magnificent informative
site.
This is really attention-grabbing, You’re an excessively professional blogger.
I’ve joined your rss feed and look forward to seeking more
of your magnificent post. Additionally, I’ve shared your web site
in my social networks
Wow, amazing blog layout! How long have you been blogging for?
you made blogging look easy. The overall look of your web site is fantastic, as well as the content!
I was suggested this web site by my cousin. I’m not sure whether this post is written by him as nobody
else know such detailed about my trouble. You’re wonderful!
Thanks!
Gambling can be of several forms, with every type requiring its legal structure.
In Nevada, for instance, there is what’s known as a”lawsuit” A suit is an agreement or a contract involving a individual placing a bet and
the individual or group placing the money at stake.
In certain countries, a”betting account” is made in which cash deposited to the account is retained by means of a bookmaker and isn’t
available to gamers; others allow online gambling but do not allow offline gambling.
Finally, you will find”rollover” trades in which the money in a player’s account is removed before it is used.
In this way, the term gambling covers a wide range
of trades and may refer to every one of these, as each has its own set of conditions
under which it can take place.
เรื่องย่อ Trinity Seven ทรินิตี้เซเว่น 7 จ้าวคัมภีร์เวท
Arata และก็สหายของเขา Kokonoe และ Mai ต่อสู้กับแม่มด
Ruberiot และก็เธอเรียกหน่วยงานขนาดยักษ์เพื่อต่อสู้กับพวกเขา Arata
และก็ Kokonoe ดำน้ำเพื่อช่วย Mai
รวมทั้งพวกเขาใช้ไม้เรียวแห่งแสงสว่างเพื่อทำลายตัวตน
หลังจากที่ Ruberiot แพ้ คุณบอกว่ามีแม่มดที่ทรงอำนาจอีกเจ็ดคนที่จะมาทำหนังสือของพวกเขา
ในฐานะนักเรียนมัธยม ผู้แสดงนำอาศัยอยู่ผู้เดียวในอพาร์ตเมนต์กระทั่งเธอได้เจอกับแมวที่ได้รับบาดเจ็บซึ่งคุณรับเลี้ยงไว้
Wow das is Good, awesome blog layout! How long have you been posting for? you make blogging look easy. The overall look of your site is super-wonderful, as well as the content unit!
бесплатный авторегер аккаунтов вк – программа цены +в интернет магазинах, linken sphere
Gambling can be of several forms, with every type requiring its legal structure.
In Nevada, for example, there is what is known as a”lawsuit” A suit
is an agreement or a contract involving a person placing
a wager and the individual or group putting the cash at stake.
In certain states, a”betting account” is created in which cash deposited into the account is kept by a bookmaker and is not
accessible to gamers; others allow online gambling but don’t allow offline gaming.
In the end, there are”rollover” trades where the cash in a player’s account is
removed before it’s used. In this way, the term gambling covers a wide range of
trades and can refer to every one of them, as each has its own set of conditions under which it
may occur.
I visited multiple websites but the audio feature for audio songs current at this web
site is truly marvelous.
Pegas – Банковский пробив,ФНС и не только!Открытие ООО, ИП.
ООО и ИП с 3-7 Банковскими счетами, кэш карты под Ваши нужды с Гарантией сохранности средств от кражи дропами.
Также Сервис “Pegas” предлагает НАДЕЖНЫЕ дебетовые карты.
Карты открываются на сканы или на живых дропов под Ваши нужды.
Работаем с большими ОБЬЁМАМИ! в неделю можем открывать до 100 карт разных Банков.
В данный момент есть много готового материала(ВТБ, АЛЬФА, HOME, ОТКРЫТИЕ, РАЙФ, МТС и тд)
Контакты:
Telegram: @PegasRUS https://t.me/PegasRUS
https://darkmoney.ac/probiv-informacii-122/pegas-bankovskii-probiv-fns-i-ne-tol-ko-243021/
газпромбанк купить дебетовую карту премиум, Пробив E-mail, Пробив по банкам, пробить счета физического лица в банках, Пробив Банк ФK Omkpыmиe, пробив сбера, пробить счет физлица, лом НДС, пробить счета физика, газпромбанк купить дебетовую карту премиум
I think this is among the most vital information for me.
And i am glad reading your article. But wanna remark on few general things, The site style is great, the articles is really
great : D. Good job, cheers
Hello just wanted to give you a quick heads up and let you know
a few of the images aren’t loading correctly. I’m not sure why but I think its a linking issue.
I’ve tried it in two different browsers and both show the same
outcome.
Игры +на xbox +one купить дешево ключи -Thief-игра-не воруй чтобы выживать а живи чтобы воровать + https://plati.market/itm/3226371
microsoft xbox +one купить игры+ https://plati.market/itm/2987570
купить игры +на xbox +one+ https://wmcentre.net/item/dirt-rally-2-0-game-of-the-year-edition-xbox-one-3205689
аккаунты xbox купить дешево+https://plati.market/itm/3116972
steam игры+http://mysel.ru/goods_info.php?id=2892901
Новые игры аккаунты в аренду+https://wmcentre.net/item/red-dead-redemption-2-xbox-one-3203361
Assassins Creed xbox one+https://plati.market/itm/2966161
Resident Evil xbox one+https://plati.market/itm/3073272
Call Of duty xbox one+https://plati.market/itm/3085414
Hitman xbox One+https://plati.market/itm/2891192
Battlefield xbox one key+https://plati.market/itm/2889815
Metro Xbox Key+https://plati.market/itm/2915157
игры XBOX XD KEY MYSEL>RU https://mysel.ru Торговая площадка цифровых товаров
FIFA 20 XBOX ONE Ключ / Цифр код + подарок
Watch Dogs 2 – Xbox Live Key –
The Crew 2 XBOX/PC+present
Diablo III: Eternal Collection Xbox One
FAR CRY
Steam Turkey 50 TL Gift Card Code(FOR TURKEY ACCOUNTS)
Netflix Турция Подарочный код 100 TL
MORTAL KOMBAT 11 XBOX ONE X/S
King?s Bounty II – Lord?s Edition XBOX ONE
Amazon Gift Card US $10
AVG TuneUp 1 ПК 1 год –
iTUNES GIFT CARD – $15(USA)
Dead Rising Triple Bundle Pack XBOX / КЛЮЧ
Thief Xbox One
Nba 2k20 xbox one
Adguard Premium 1ПК+https://wmcentre.net/item/adguard-premium-1pk-na-1-god-3203400
AVG TuneUp 1 ПК 1 ключ+https://plati.market/itm/3048052
Хочешь купить машину, срочно нужны деньги, не хватате на покупку иди в банк HOME BANKE
Покупай на ENOT-способ оплаты(0% при оплате банковской картой)11 способов оплаты
Its such as you read my thoughts! You appear to grasp a lot about this, such as you wrote the
e-book in it or something. I feel that you just can do with
some percent to drive the message house a bit, but instead of that, that is wonderful blog.
A fantastic read. I will definitely be back.
If you want to increase your knowledge only keep visiting
this web site and be updated with the hottest news update
posted here.
Betting can be of several forms, with every type requiring its own legal
arrangement. In Nevada, for instance, there is what is
known as a”lawsuit” A lawsuit is an agreement or a contract between a individual placing a bet and the person or group placing the money at stake.
In some states, a”betting account” is created in which
cash deposited to the account is kept by means of a bookmaker
and isn’t available to gamers; others let online gambling but don’t permit offline gambling.
In the end, you will find”rollover” transactions where the
money in a player’s account is removed before it’s
used. This manner, the term gambling covers a vast range of transactions and may refer to every one of them,
as each has its own set of circumstances under which it can occur.
Hi mates, how is everything, and what you would like
to say about this article, in my view its actually awesome for me.
You should take part in a contest for one of the highest quality blogs
on the internet. I will recommend this site!
It’s really a nice and useful piece of information. I’m satisfied that you just shared this useful information with us.
Please keep us informed like this. Thanks for sharing.
Howdy! Quick question that’s completely off topic.
Do you know how to make your site mobile friendly?
My weblog looks weird when viewing from my iphone 4.
I’m trying to find a theme or plugin that might be able to correct this
issue. If you have any suggestions, please share.
Many thanks!
Hello there! I could have sworn I’ve visited this web site before but after browsing through many of the articles I realized it’s new to me. Anyhow, I’m definitely delighted I found it and I’ll be book-marking it and checking back frequently!
Excellent weblog here! Additionally your web site rather a lot up very fast!
What web host are you using? Can I get your affiliate hyperlink in your host?
I desire my website loaded up as fast as yours lol
I’ve been browsing on-line more than 3 hours these days, yet I by no means discovered any interesting article like yours.
It’s pretty worth sufficient for me. In my opinion, if all
site owners and bloggers made good content as you did,
the web will likely be a lot more helpful than ever before.
nice stuff you have posted here.. it seems you have put great effort in writing this
You could definitely see your skills within the article you write.
The sector hopes for even more passionate writers like you
who aren’t afraid to say how they believe. All the time follow your heart.
It’s an awesome post for all the online viewers; they will obtain benefit
from it I am sure.
Your method of describing everything in this post is
actually nice, every one can simply understand it, Thanks a lot.
Betting can be of several types, with every type requiring its
own legal structure. In Nevada, for instance, there is what’s known as a”lawsuit” A lawsuit is an agreement or a
contract involving a individual placing a wager and the
individual or group placing the money at stake. In certain countries, a”betting account” is created in which money deposited to the
account is retained by a bookmaker and isn’t available to players;
others let online gambling but do not allow offline gambling.
Finally, there are”rollover” transactions where the money in a player’s
account is withdrawn before it is used. This way, the term gaming covers a
vast selection of trades and may refer to every
one of them, as each has its own set of conditions under
which it can occur.
Excellent post. Keep writing such kind of info on your site.
Im really impressed by your site.
Hello there, You’ve performed a great job. I will certainly digg
it and personally recommend to my friends. I’m sure they will be benefited from this website.
An outstanding share! I have just forwarded this onto a
coworker who had been conducting a little research on this.
And he actually ordered me lunch simply because I found
it for him… lol. So let me reword this….
Thank YOU for the meal!! But yeah, thanx for spending time to discuss this subject here on your site.
WOW just what I was looking for. Came here by
searching for http://post.12gates.net/member.php?action=profile&uid=210629
It’s amazing to visit this website and reading the views of all friends about this article, while I am also eager of getting know-how.
Wow, that’s what I was searching for, what a
stuff! present here at this website, thanks admin of this website.
Gambling can be of many forms, with every type requiring its legal arrangement.
In Nevada, for example, there is what is known as a”lawsuit” A lawsuit
is an agreement or a contract involving a person placing a wager and the person or group putting the money at
stake. In some countries, a”gaming accounts” is made in which cash deposited to the account is retained
by a bookmaker and is not available to gamers; others let online gambling but don’t
allow offline gambling. Finally, there are”rollover” trades where the money in a participant’s account is removed before it
is used. In this way, the expression gaming covers a wide range of trades and can refer to every one of them, as each has its own set
of circumstances under which it can occur.
Excellent goods from you, man. I’ve understand your stuff previous
to and you’re just too excellent. I actually like what you
have acquired here, really like what you’re saying and the way in which you
say it. You make it enjoyable and you still take care of to keep it smart.
I can not wait to read much more from you. This is really a wonderful site.
Incredible points. Solid arguments. Keep up the amazing work.
What’s up, every time i used to check webpage posts here early in the
daylight, for the reason that i like to learn more and more.
excellent points altogether, you simply gained a new reader.
What might you recommend about your publish that you just made some days ago?
Any positive?
Sweet blog! I found it while searching on Yahoo News. Do you have
any tips on how to get listed in Yahoo News? I’ve been trying for a
while but I never seem to get there! Many thanks
Howdy! This post couldn’t be written any better!
Looking through this post reminds me of my previous roommate!
He constantly kept talking about this. I am going to send this information to him.
Fairly certain he will have a very good read. I appreciate you for sharing!
When some one searches for his required thing, thus he/she wants to be available that in detail, so that thing is maintained over here.
I always used to study paragraph in news papers but now as
I am a user of internet therefore from now I am using net for articles,
thanks to web.
I love reading a post that can make men and women think. Also, many thanks for allowing for me to comment!
After exploring a handful of the articles on your web site, I
really appreciate your technique of writing a blog.
I book-marked it to my bookmark webpage list and will be checking back soon. Take a look at my web site too and
tell me how you feel.
You’re so awesome! I do not think I’ve truly read through
something like this before. So nice to discover somebody with original thoughts on this subject.
Seriously.. thanks for starting this up. This site is one thing
that is required on the web, someone with some originality!
I read this paragraph fully about the difference of most recent and preceding technologies, it’s awesome article.
Woah! I’m really digging the template/theme of
this site. It’s simple, yet effective. A lot of times it’s challenging to
get that “perfect balance” between usability and visual appeal.
I must say you have done a very good job with this.
Also, the blog loads super quick for me on Internet explorer.
Superb Blog!
Thanks for sharing your info. I really appreciate your efforts and
I am waiting for your further write ups thanks once again.
Your mode of telling all in this paragraph is actually nice, every one be able to effortlessly understand it, Thanks a lot.
Gambling can be of many types, with every type requiring its
legal arrangement. In Nevada, for instance, there is what’s called a”suit.” A lawsuit is
an agreement or a contract involving a person placing a bet and the individual or group putting
the cash at stake. In certain states, a”betting account” is created in which
cash deposited into the account is kept by means of a
bookmaker and isn’t available to players; others allow online gambling but don’t allow offline gambling.
Finally, you will find”rollover” transactions in which the cash in a participant’s account
is removed before it’s used. This way, the term
gambling covers a wide range of trades and may refer to
all of these, as each has its own set of circumstances under which it may take place.
I pay a visit everyday a few websites and blogs to read content, however this weblog provides quality based posts.
Вывод средств
Подробнее по ссылке: https://forms.yandex.ru/u/610fe0c0a7a9d9645645/success/72126?AAAAAinsidetheclinic.comBBBBB
Its like you read my mind! You seem to know a lot about this, like you wrote the book in it or something.
I think that you can do with a few pics to
drive the message home a little bit, but other than that, this is
fantastic blog. An excellent read. I will definitely
be back.
This paragraph gives clear idea designed for the new people of blogging,
that actually how to do blogging.
spreading how much ivermectin to give a dog with mange
ozawodowi is stromectol ivermectin
order ivermectin 3mg
– coronavirus ivermectin
http://ivermectin-12mg.net/# – buy oral ivermectin
niebajest what to expect after taking ivermectin for scabies
We are excited to have stumbled across your site, it’s exactly the thing people from work were lookiin for constantly in search of. The detailed information here on the nice website is always specialized and will help my clients quite a lot one of kind help. Looks like everone on the site gains incredible amounts of info about subjects on the site and the other hyper links and info definitely are evident. I am not on the internet all day long so as I get a chance We are totally scouring this sort of information and things closely exactly like it. Cheers. If you needed major services like: trademark lawyer illinois also Scottsdale and Phoenix website design near me in 86011 I can help.
I do not even know how I ended up here, but I thought this post was
good. I don’t know who you are but definitely you’re going
to a famous blogger if you aren’t already 😉 Cheers!
Very interesting points you have noted, regards for putting up.
my homepage – seo packages uk
https://tipsforperfectinterview.com
These are truly great ideas in regarding blogging.
You have touched some pleasant points here. Any way
keep up wrinting.
If some one desires expert view on the topic of blogging after that i recommend him/her to go to see this website, Keep up the good work.
Hello There. I found your weblog the usage of msn.
This is a really well written article. I will make sure to bookmark it and return to read more of your helpful information. Thank you
for the post. I will certainly comeback.
Hi there to all, the contents existing at this site
are genuinely remarkable for people knowledge, well, keep up the nice work fellows.
Do you have a spam issue on this site; I also am a blogger, and I was curious about your situation; many
of us have created some nice methods and we are looking to trade solutions with
other folks, why not shoot me an e-mail if interested.
This paragraph is genuinely a fastidious one it helps new web viewers, who are wishing for blogging.
Oh my goodness! Incredible article dude! Thanks, However I am going through issues with your RSS.
I don’t know the reason why I am unable to join it.
Is there anybody getting similar RSS problems? Anyone who knows the solution will you kindly respond?
Thanx!!
I know this site presents quality depending posts and extra material, is there
any other web page which gives these data in quality?
Genuinely when someone doesn’t understand afterward its up to
other people that they will assist, so here it happens.
Hi, i think that i saw you visited my site so
i came to “return the favorâ€.I am trying to find things
to enhance my website!I suppose its ok to use a few of your ideas!!
It’s hard to find knowledgeable people in this particular subject, but you sound like you know what you’re talking about!
Thanks
I loved as much as you’ll receive carried out right here.
The sketch is tasteful, your authored subject matter stylish.
nonetheless, you command get got an impatience over that you
wish be delivering the following. unwell unquestionably come more formerly again since exactly the
same nearly a lot often inside case you shield this
hike.
I am actually grateful to the owner of this web site who has shared this wonderful article at
at this place.
Appreciate this post. Will try it out.http://metodbox.org/user/StarSes/
Hello! Would you mind if I share your blog with my myspace group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Many thanks
Great post. I used to be checking continuously this weblog and I’m inspired! Very useful information particularly the remaining part 🙂 I deal with such info a lot. I used to be seeking this certain information for a long time. Thank you and good luck. http://hmfc.ru/index.php?subaction=userinfo&user=etuzu
Hello to every one, the contents present at this website are genuinely awesome for people experience, well, keep up the good work fellows. http://m-power.ru/forum/memberlist.php?&pp=50&order=desc&sort=posts<r=I&page=11
Hiya very nice blog!! Man .. Excellent .. Wonderful .. I will bookmark your website and take the feeds additionally? I’m glad to search out so many helpful information right here in the post, we’d like work out extra strategies in this regard, thanks for sharing. . . . . . http://forum.bashtel.ru/showthread.php?p=2049498&mode=threaded
Pretty great post. I just stumbled upon your weblog and wanted to say
that I’ve really enjoyed surfing around your blog posts.
After all I will be subscribing to your feed and I’m hoping you write again very
soon!
I have read so many content on the topic of the blogger lovers but this paragraph is really a good post, keep it up. https://topseochecker.com/tury5.ru
This is my first time pay a visit at here and i am truly impressed to read all at alone place. https://www.forum.omskmama.ru/viewtopic.php?p=10723766
Aw, this was a really good post. Finding the time and actual effort to generate a really good article… but what can I say… I hesitate a whole lot and don’t manage to get anything done.
Wow, incredible weblog structure! How lengthy have you been running a blog for? you made running a blog look easy. The full look of your site is wonderful, let alone the content!
https://crimea-kurort.com/side/221-otdih_v_rossii/1650
check out here crypto loan without collateral
I’m really enjoying the design and layout of your website. It’s a very easy on the eyes which makes it much more pleasant for me to come here and visit more often. Did you hire out a developer to create your theme? Fantastic work! http://www.carters.bb/priv_stats/usage_202006.html
This paragraph provides clear idea for the new people of
blogging, that truly how to do blogging and site-building.
These are truly wonderful ideas in regarding blogging. You have touched some pleasant points here. Any way keep up wrinting. http://idm-group.ru/talk/forum/vecherinki/6801.html
It’s really a nice and helpful piece of information. I am satisfied that you just shared this helpful information with us. Please stay us informed like this. Thank you for sharing. http://bc-tremonia.de/usage/bc-tremonia_de/usage_202007.html
Hi friends, good post and fastidious arguments commented
here, I am actually enjoying by these.
Having read this I thought it was really informative. I appreciate you spending some time and effort to put this short article together. I once again find myself spending a lot of time both reading and posting comments. But so what, it was still worthwhile! http://www.hmcity.ru/communication/forum/user/105860/
I every time used to read piece of writing in news papers but now as I am a user of internet so from now I am using net for articles or reviews, thanks to web.http://www.civfanatics.ru/members/242834-starVon
http://k636419q.beget.tech/index.php?subaction=userinfo&user=izetinyj
I loved as much as you will receive carried out right here. The sketch is attractive, your authored material stylish. nonetheless, you command get bought an edginess over that you wish be delivering the following. unwell unquestionably come more formerly again since exactly the same nearly a lot often inside case you shield this increase.
https://forum.cryptoff.org/index.php?/topic/12099-exchangesumo-monitoring-obmennykh-punktov-elektronnykh-va/
Hello There. I found your weblog using msn. This is a really
well written article. I’ll make sure to bookmark it and come back to learn more of your helpful info.
Thanks for the post. I’ll definitely return.
Hi this is somewhat of off topic but I was wanting to know if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding expertise so I wanted to get advice from someone with experience. Any help would be greatly appreciated! http://cuckoo-club.ru/memberlist.php?first_char=&start=41650
http://cuckoo-club.ru/memberlist.php?start=1300&sk=a&sd=d
http://www.cuckoo-club.ru/memberlist.php?sk=d&sd=a&first_char=&mode=searchuser&start=39625
http://www.cuckoo-club.ru/memberlist.php?sk=a&sd=d&start=1300
http://www.cuckoo-club.ru/memberlist.php?sk=c&sd=a&first_char=&start=41350
https://www.fpv1.ru/member.php?2475-ykosi&tab=activitystream&type=user&page=21
Hi there, I enjoy reading through your article post.
I wanted to write a little comment to support you.
Gambling can be of several forms, with each type
requiring its own legal arrangement. In Nevada, for
instance, there is what is known as a”suit.” A suit is an agreement or a contract between a
individual placing a wager and the person or group
placing the money at stake. In certain countries, a”betting account” is created in which money
deposited into the account is kept by means of a bookmaker and isn’t accessible to gamers; others let online gambling
but do not allow offline gaming. Finally, there are”rollover” transactions where the cash
in a player’s account is removed before it’s used. In this
way, the expression gambling covers a vast range of trades and
can refer to all of these, as each has its own set of circumstances under which it
may take place.
Betting can be of many types, with every type requiring
its legal arrangement. In Nevada, for instance, there is what is known as a”suit.” A lawsuit is an agreement or a contract involving a individual placing a bet and
the person or group putting the money at stake.
In some countries, a”gaming accounts” is created in which cash
deposited to the account is kept by means of a bookmaker and
isn’t available to players; others let online gambling but don’t permit offline gambling.
In the end, there are”rollover” trades in which the money in a participant’s account is removed before it’s used.
In this way, the term gambling covers a
vast selection of trades and can refer to every one of them, as each has its own set of circumstances
under which it can occur.
http://harraseeketlunchandlobster.com/webalizer/usage_202101.html
https://drvisual.be/plesk-stat/webstat/usage_202011.html
http://www.seowatchdog.club/it/www/beautifulandhappy.ru
http://guywhosingshigh.com/plesk-stat/webstat/usage_202101.html
https://www.langerent.com/webalizer/usage_202012.html
After going over a handful of the blog posts on your web site, I truly like your technique of writing a blog. I book marked it to my bookmark webpage list and will be checking back soon. Take a look at my web site as well and tell me how you feel. http://seexxxnow.net/index.php?subaction=userinfo&user=usajevo
Hello There. I discovered your weblog the use of msn. That is a really neatly written article.
I will be sure to bookmark it and come back to read more of your helpful
info. Thanks for the post. I’ll definitely return.
Post writing is also a excitement, if you be acquainted with then you can write otherwise it is complicated to
write.
Highly descriptive post, I liked that bit. Will there be a part 2? http://forum.l2c4.com/member.php?u=11488
I’m extremely impressed together with your writing talents as well as with the layout in your weblog. Is this a paid subject matter or did you modify it your self? Either way keep up the nice high quality writing, it’s rare to look a great blog like this one nowadays.. http://footwear.ua/forum/index.php?act=morelist&id_parent=23264&id_group=5&offset_detail=0
No matter if some one searches for his required thing, therefore he/she wishes to be available that in detail, thus that thing is maintained over here. https://prlog.ru/analysis/tury5.ru
Marvelous, what a website it is! This webpage presents helpful data to
us, keep it up.
No matter if some one searches for his necessary thing, therefore he/she wants to be available that in detail, thus that thing is maintained over here. https://rech-agent.ru/cruise/cruisedetails/sankt-peterburg_2955.html
Excellent blog here! Also your web site loads up
very fast! What host are you using? Can I get your
affiliate link to your host? I wish my site loaded up as fast as yours lol
Hi there Dear, are you truly visiting this website daily, if so after that you will absolutely get good knowledge. http://forum.russsia.ru/lofiversion/index.php/t20209.html
I am not sure where you’re getting your info, but good topic. I needs to spend some time learning more or understanding more. Thanks for excellent info I was looking for this information for my mission. http://loreundleo.at/plesk-stat/webstat/usage_202005.html
Hi there! I could have sworn I’ve been to this blog before but after browsing through some of the
post I realized it’s new to me. Anyways, I’m definitely happy I found it
and I’ll be book-marking and checking back frequently!
What’s up mates, good article and nice arguments commented at this place, I am really enjoying by these. http://www.artinfo.ru/ru/news/main/artarchive/contents-46.htm
Please let me know if you’re looking for a author for your site.
You have some really good posts and I feel I would be a good asset.
If you ever want to take some of the load off, I’d really
like to write some articles for your blog in exchange for a link
back to mine. Please shoot me an email if interested. Kudos!
Somebody necessarily assist to make seriously articles I would state. That is the first time I frequented your web page and so far? I surprised with the analysis you made to create this particular post extraordinary. Excellent task! http://nisus-eng.com/stats/usage_202006.html
Hey there, I think your site might be having browser compatibility issues.
When I look at your blog site in Safari, it looks fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up! Other then that, great blog!
all the time i used to read smaller articles or
reviews that also clear their motive, and that is also happening with this paragraph which I am reading at this place.
Very good post. I am facing many of these issues as well..
Thanks for one’s marvelous posting! I quite enjoyed reading it, you’re a great author.I will ensure that I bookmark your blog and may come back at some point. I want to encourage you to continue your great writing, have a nice weekend! http://avangardplastik.ru/index.php?subaction=userinfo&user=uryna
Helpful info. Fortunate me I discovered your web site by accident, and I’m shocked why this twist of fate did not took place in advance! I bookmarked it.http://galeevmm.ru/forum/memberlist.php?mode=viewprofile&u=316778
http://pravoznavec.com.ua/partners/profile/ipivamafy-8843.html
Hi there, just became alert to your blog through Google, and found that it’s truly informative. I’m going to watch out for brussels. I will appreciate if you continue this in future. Many people will be benefited from your writing. Cheers!
http://sql-tutorial.ru/ru/tag/%F1%E0%EC%EE%F1%EE%E5%E4%E8%ED%E5%ED%E8%E5.html
Does your website have a contact page? I’m
having problems locating it but, I’d like to send you an email.
I’ve got some recommendations for your blog you might
be interested in hearing. Either way, great site and I look forward to seeing it develop over time.
https://sumkin.ru/forum/member.php?u=13434
http://m-power.ru/forum/memberlist.php?&pp=100&order=asc&sort=username<r=Y&page=2
https://www.fpv1.ru/member.php?2475-ykosi&tab=activitystream&type=photos&page=9
https://www.fpv1.ru/member.php?2475-ykosi&tab=activitystream&type=all&page=8
http://www.cuckoo-club.ru/memberlist.php?start=39625&sk=d&sd=a
http://ebc-koeln.de/usage/usage_202101.html
https://www.towshop.com/webalizer/usage_202009.html
https://seocheck.biz/pt/www/beautifulandhappy.ru
http://oldtimer-paradies.de/usage/usage_202011.html
http://www.fashionwiredaily.com/html/usage/usage_202012.html
Great article.
Hmm is anyone else having problems with the images on this blog loading?
I’m trying to determine if its a problem on my end or if it’s the blog.
Any responses would be greatly appreciated.
Thanks to my father who stated to me on the topic of this weblog, this website is genuinely amazing.
Thank you for sharing your info. I truly appreciate your efforts and I am waiting for your
next write ups thank you once again.
Today, while I was at work, my sister stole my iPad and tested to see if
it can survive a 30 foot drop, just so she
can be a youtube sensation. My apple ipad is now destroyed
and she has 83 views. I know this is completely off topic but I had to share it with someone!
Fine way of telling, and pleasant post to take data regarding my presentation focus, which i am going to deliver in institution of higher education. http://hkbad.com.ua/index.php?subaction=userinfo&user=efedef
Hi i am kavin, its my first occasion to commenting anyplace,
when i read this article i thought i could also make comment due to
this sensible article.
I was able to find good information from your blog articles.
I’m impressed, I must say. Seldom do I encounter a
blog that’s both educative and interesting, and let me tell you, you’ve hit the nail on the head.
The problem is something that not enough people are speaking
intelligently about. Now i’m very happy I came across this during my hunt for
something regarding this.
It is in reality a great and useful piece of info.
I am satisfied that you shared this helpful
information with us. Please keep us up to date like this. Thank you for sharing.
Attractive section of content. I just stumbled upon your web site
and in accession capital to assert that I acquire actually enjoyed account your blog posts.
Any way I’ll be subscribing to your feeds and even I achievement
you access consistently fast.
Lastly weighed in on a free no lose wager the Cowboys will win. Exodus extra to guess
with small particulars to create your account to check.
If all your cash and run they won’t abuse your checking account.
Whether this usually takes into account. With sports activities bettors encounter
the company’s income growing to 750 million in 2022 and then enroll.
It permits people who ask US all to enroll with the
bookmaker webpage is easy. States already
earned themselves as you’d need to pay the bookmaker
the vig. As sports betting operators have a site that will provide special bets for.
Which are the statutory authority to conduct and manage single-event sports betting in India
is now. Bettingjobs is the worldwide betting in India. Safety of your
particulars to create a risky atmosphere in terms of sports betting.
Safety some books don’t should but the skins
will also be adopted. Quick payouts get cash as your reward
once you solely should threat 130 and will win. Betting sites may
yield high potential payouts as such payouts can try again.
It is in reality a great and useful piece of
info. I’m happy that you shared this helpful information with us.
Please keep us up to date like this. Thank you
for sharing.
Tremendous things here. I’m very satisfied to peer your
post. Thank you a lot and I am looking ahead to touch you.
Will you please drop me a mail?
I think the admin of this website is actually working
hard in favor of his website, because here every stuff is quality based material.
Перейти на сайт: http://s-felichita.ru/index.php?subaction=userinfo&user=uqizese
Перейти на сайт: http://wkrotce.pl/profile.php?id=6&user=392741
Betting can be of several types, with every type requiring its legal arrangement.
In Nevada, for example, there is what is called a”lawsuit” A suit is an agreement
or a contract involving a person placing a bet and the individual or group putting the money at stake.
In some states, a”gaming accounts” is created in which
cash deposited into the account is kept by means of
a bookmaker and isn’t accessible to players; others let online gambling but don’t permit offline gambling.
Finally, you will find”rollover” trades in which the cash in a participant’s account is removed before it is used.
This manner, the term gaming covers a wide selection of trades and
may refer to every one of them, as each has its own set of
conditions under which it may take place.
Перейти на сайт: http://pautinka.ch.ua/index.php?subaction=userinfo&user=ehizejiw
I savor, cause I found exactly what I was taking a look for.
You have ended my 4 day long hunt! God Bless you man. Have a nice day.
Bye
Excellent beat ! I wish to apprentice while
you amend your website, how could i subscribe
for a blog website? The account helped me a appropriate deal.
I had been a little bit familiar of this your broadcast offered vibrant transparent idea
Greetings! Very helpful advice in this particular article!
It’s the little changes that will make the most
important changes. Many thanks for sharing!
certainly like your web site however you need to check the
spelling on quite a few of your posts. Several of them are rife with spelling
issues and I in finding it very bothersome to tell the reality on the other hand
I will definitely come again again.
Do you mind if I quote a few of your posts as long as I provide credit and sources back to your blog? My blog site is in the exact same niche as yours and my visitors would genuinely benefit from a lot of the information you present here. Please let me know if this okay with you. Cheers!
https://marketinsightsl.com/community/profile/nicole/
Excellent way of telling, and pleasant post to
obtain data regarding my presentation focus, which i am going to present in college.
dawning ivermectin powder
netsains stromectol prescription
buy ivermectin 3 mg tablets
– stromectol oral
http://ivermectin-12mg.net/# – ivermectin 3mg tablets price
accentuent how to treat stromectol hives
It’s the best time to make a few plans for the future and it’s time to be happy. I have learn this publish and if I may just I desire to recommend you some attention-grabbing issues or suggestions. Perhaps you can write next articles relating to this article. I desire to learn even more things about it!
https://landscaperjakarta.com/community/profile/dana/
Thank you for the good writeup. It in fact was a amusement account it.
Look advanced to far added agreeable from you!
By the way, how could we communicate?
This is my first time go to see at here and i am in fact
happy to read everthing at single place.
What i do not understood is if truth be told how you
are now not actually much more well-favored than you might be now.
You are so intelligent. You understand thus considerably relating to this
topic, made me personally consider it from numerous various angles.
Its like men and women aren’t fascinated unless
it is one thing to do with Girl gaga! Your individual stuffs great.
All the time deal with it up!
Thanks for sharing your thoughts about https://spamdb.science/wiki/Book_Is_Sure_To_Make_An_Impression_In_What_You_Are_Promoting. Regards
Very good blog! Do you have any hints for aspiring writers?
I’m planning to start my own blog soon but I’m a little lost on everything.
Would you suggest starting with a free platform like WordPress or go for a paid option? There are so many
choices out there that I’m totally overwhelmed .. Any suggestions?
Cheers!
Ever considering that the casinos began appearing in metropolitan areas round
the Earth, folks happen to be searching for strategies
to win. They come across this not only a challenge but in addition a source of passion. And why don’t
you? Playing a casino match provides the prospect of getting something
for nothing and there usually are a great deal of people
keen to pay out cash to receive the best cards or combinations.
So, individuals will do just about everything to
understand to triumph casino matches.
One major things concerning casino game titles
is that they are about probabilities. That is certainly why casino proprietors insist on earning bets
open to gamers. If you win then you can claim your winnings, of course, if you lose then you have to simply
take more stakes. The more bets you take from, the more larger
the losses you have to generate. The cut card roulette and blackjack is just one other way to lose.
What exactly is really intriguing about winning in casino gaming?
Besides the thrill of competition, the adventure of winning attracts a specific
pride to this particular person who has pulled off it.
Achieving something through sheer chance or even through a few clever approach is a intriguing idea.
In a nutshell, profitable roulette, blackjack or even any one of another casino matches can offer the person who has
reached it immense pleasure and pride.
Roulette and Texas maintain Celtics are just two of their absolute most well-known video online games.
Blackjack and poker are also popular. The important point about those games will be the outcome is dependent up on the last two numbers
that have been dealt with you, especially, the quantity of your arms
(theces) and also the range of one’s threes (punches).
From the Texas maintain ’em and the casino variant,
the winning jackpot, which is named the flop, is thirty seven, whilst in the roulette variant,
it’s thirty-six.
Thanks for finally writing about > Tinea versicolor –
pictures, symptoms, causes, treatment < Loved it!
This information is invaluable. How can I find out more?
Attractive component to content. I just stumbled upon your website and
in accession capital to claim that I get in fact enjoyed account your blog posts.
Any way I’ll be subscribing on your feeds and even I achievement you get admission to consistently
quickly.
Yes! Finally something about abroadsanjal.com.
Touche. Great arguments. Keep up the great spirit.
Greetings from Ohio! I’m bored at work so I decided to check out your website on my iphone during lunch break.
I love the info you present here and can’t wait to take a look when I
get home. I’m amazed at how quick your blog loaded on my phone ..
I’m not even using WIFI, just 3G .. Anyways, fantastic site!
This post is really a pleasant one it helps new internet people, who are wishing for blogging.
I read this article completely about the comparison of most recent and
earlier technologies, it’s remarkable article.
This text is worth everyone’s attention. When can I
find out more?
Your style is so unique in comparison to other people I have read stuff from.
Many thanks for posting when you’ve got the
opportunity, Guess I’ll just book mark this site.
Wow, amazing blog structure! How lengthy have you ever been blogging
for? you made blogging glance easy. The entire look of your web site is great,
as neatly as the content!
Hey there just wanted to give you a quick heads up. The text in your
content seem to be running off the screen in Firefox.
I’m not sure if this is a format issue or something to do with internet browser compatibility but I thought I’d post to let you know.
The style and design look great though! Hope you get
the problem solved soon. Cheers
Howdy this is kind of of off topic but I was wondering if blogs use WYSIWYG editors or if you have to manually code
with HTML. I’m starting a blog soon but have no coding
knowledge so I wanted to get guidance from someone with experience.
Any help would be greatly appreciated!
We’re a group of volunteers and starting a new scheme in our community.
Your site offered us with valuable information to work on. You have done a formidable job and
our entire community will be thankful to you.
Everything wrote made a great deal of sense.
But, think about this, what if you added a little content?
I ain’t saying your content is not good, but what if you added a title that grabbed folk’s
attention? I mean Tinea versicolor – pictures, symptoms, causes, treatment is kinda boring.
You might look at Yahoo’s home page and see how they write article titles to
grab people interested. You might add a video or a related
pic or two to get people interested about what you’ve got
to say. Just my opinion, it would make your posts a little livelier.
Great blog right here! Additionally your web site rather a lot
up fast! What host are you the use of? Can I get your affiliate link for your host?
I want my site loaded up as quickly as yours lol
Betting can be of many types, with each type requiring
its legal structure. In Nevada, for example,
there is what is known as a”suit.” A lawsuit is an agreement or a contract involving a individual placing a wager and the individual or group
putting the money at stake. In some states, a”gaming accounts” is created in which money deposited to
the account is kept by a bookmaker and is not accessible to players; others let online
gambling but don’t permit offline gaming. In the end,
you will find”rollover” transactions where the cash in a player’s account is withdrawn before it is
used. This manner, the expression gaming covers a wide range of transactions and can refer to
every one of these, as each has its own set
of conditions under which it may take place.
You are so interesting! I do not suppose I’ve truly read anything like this before.
So good to discover somebody with a few unique thoughts on this
subject matter. Seriously.. thanks for starting this up.
This website is something that’s needed on the internet, someone with some originality!
Today, while I was at work, my cousin stole my iphone and tested to see if it
can survive a thirty foot drop, just so she can be a youtube sensation. My apple
ipad is now destroyed and she has 83 views. I know this is totally off topic but I had to share it with
someone!
Great website. Plenty of helpful info here. I’m sending it to
several friends ans also sharing in delicious. And obviously, thank you
in your effort!
Betting can be of many types, with each type requiring its own legal arrangement.
In Nevada, for example, there is what is known as a”suit.”
A lawsuit is an agreement or a contract involving a person placing
a wager and the person or group putting the cash at stake.
In some states, a”gaming accounts” is created in which cash deposited into the account is retained by means of a bookmaker and is not available to gamers; others let online gambling but
don’t allow offline gaming. Finally, there are”rollover” transactions where the cash in a participant’s account is withdrawn before it is used.
In this manner, the expression gambling covers a vast selection of trades and can refer to all of these,
as each has its own set of circumstances under which it
may occur.
Hi mates, its enormous article about cultureand entirely explained, keep
it up all the time.
This is very interesting, You are a very skilled blogger.
I’ve joined your rss feed and look forward to seeking more
of your wonderful post. Also, I’ve shared your website in my
social networks!
Very nice post. I just stumbled upon your weblog and wanted
to say that I’ve truly enjoyed surfing around your blog posts.
After all I’ll be subscribing to your feed and I hope you write again soon!
Nice post. I used to be checking constantly this weblog and I
am impressed! Extremely helpful information specifically the ultimate part 🙂 I deal with such
information a lot. I was looking for this particular info
for a very long time. Thanks and best of luck.
I do not know if it’s just me or if perhaps everybody else encountering problems with your blog.
It looks like some of the written text in your content are
running off the screen. Can somebody else please provide feedback and let me know if this is happening to them as well?
This could be a problem with my internet browser because I’ve had this happen before.
Appreciate it
Thanks for the marvelous posting! I actually enjoyed reading it, you happen to
be a great author. I will make certain to
bookmark your blog and will come back very soon. I
want to encourage yourself to continue your great posts,
have a nice morning!
I really like your blog.. very nice colors & theme.
Did you design this website yourself or did you
hire someone to do it for you? Plz respond as I’m looking to
construct my own blog and would like to know where u got this from.
thanks a lot
Very shortly this site will be famous amid all blogging people, due to it’s good articles
I simply couldn’t depart your site before suggesting that I really enjoyed the standard information a person supply
in your visitors? Is going to be again steadily in order to check up on new posts
I’m amazed, I have to admit. Seldom do I encounter a blog
that’s both educative and interesting, and without
a doubt, you’ve hit the nail on the head. The issue is an issue that
too few men and women are speaking intelligently about. I am very happy I stumbled across this in my
search for something concerning this.
all the time i used to read smaller articles or reviews which as well clear
their motive, and that is also happening with this paragraph which I
am reading at this place.
Hello i am kavin, its my first time to commenting anyplace, when i read this article i thought i could also make comment due to this good paragraph.
Excellent post. I was checking continuously this blog and
I’m impressed! Extremely helpful information specially
the last part 🙂 I care for such info a lot. I was seeking this particular
info for a very long time. Thank you and good luck.
Hi! I could have sworn I’ve been to this website before but after reading through some of the post I realized it’s new to me.
Anyhow, I’m definitely delighted I found it and I’ll be bookmarking and checking
back frequently!
Wow, awesome blog layout! How long have you been blogging for?
you made blogging look easy. The overall look of your website is great, as well as the content!
Betting can be of several forms, with every type requiring its own legal structure.
In Nevada, for example, there is what’s called a”lawsuit” A suit is an agreement or a contract
between a individual placing a bet and the person or group putting the
money at stake. In certain countries, a”gaming accounts” is created in which cash deposited into the account
is kept by a bookmaker and isn’t available to players; others let online gambling but do not allow
offline gaming. Finally, there are”rollover” trades in which the money in a participant’s account
is removed before it is used. In this way, the expression gambling
covers a wide range of trades and may refer to every one
of these, as each has its own set of circumstances under which it can occur.
Definitely believe that which you said. Your favorite reason appeared to be on the internet the simplest thing to be
aware of. I say to you, I certainly get irked while people consider worries that they plainly
don’t know about. You managed to hit the nail upon the top as well as defined
out the whole thing without having side-effects ,
people could take a signal. Will probably be back to get more.
Thanks
TPE & Silicone Love Dolls
male sex doll
I don’t know whether it’s just me or if perhaps everyone else encountering
issues with your site. It seems like some of the written text within your content are
running off the screen. Can someone else please comment and let me know if this is happening to them too?
This may be a issue with my browser because I’ve had this happen before.
Appreciate it
http://ubezpieczenieauta.com.pl http://ubezpieczeniabielsko.pl http://ubezpieczenie-dziecka.pl https://Bit.ly/3G4WJbU https://tinyurl.com/kkrh5ppj http://allianz-ubezpieczenia.pl https://bit.ly/3Htrjfr https://bit.ly/3G9PHTf https://cutt.ly/sRAzgRD https://tinyurl.com/6vhv3br8 http://ubezpieczeniaaut.com.pl http://Szybkie-Ubezpieczenia.pl/ http://fart-ubezpieczenia.pl https://bit.ly/3Gf2Fz2 https://cutt.ly/rUTSShP https://tinyurl.com/bbhm4pye https://tinyurl.com/zfssp7nr https://bit.ly/3b2GSMI https://cutt.ly/FRAzfuD https://tinyurl.com/2yjjx9yv http://ubezpieczenia-ranking.pl
Very great post. I just stumbled upon your blog and wished to mention that
I’ve really enjoyed surfing around your weblog posts. In any case I’ll
be subscribing in your feed and I hope you write once more
soon!
http://lekkie-pioro.pl http://pier-agence.com http://tpzlun.pl http://bannedcd.org http://pepsiohyesabhi.com http://adelewashere.com http://tomaszkubis.pl http://englishwebteachers.com http://mpfasdpic.org http://3az.pl http://kerganos.com http://perfect-meble.pl http://ecceo13-iof.org http://jnbfgk.com http://birchclothing.com Demands ought to not be sent to the Information Commissioner’s Workplace (ICO), other than where
the requester wants info the ICO holds.
Hi, I do think this is an excellent website.
I stumbledupon it 😉 I’m going to return yet
again since I saved as a favorite it. Money and freedom is the best way to change,
may you be rich and continue to help other people.
http://datoura.org http://firefoxstory.com http://softcupbra.org http://mna-sf.org http://jadalive.org http://emtec-group.com.pl http://szalonypodroznik.pl http://researchmarket24.com http://urbantraffic.pl http://woco.pl http://constitutionfair.org http://lubsacro.pl
Hi there, just became aware of your blog through Google, and found that it’s really informative.
I am gonna watch out for brussels. I’ll appreciate if you
continue this in future. A lot of people will be benefited
from your writing. Cheers!
It’s awesome for me to have a site, which is valuable designed
for my experience. thanks admin
Hi there, i read your blog from time to time and i own a similar one and
i was just curious if you get a lot of spam feedback?
If so how do you reduce it, any plugin or anything you can suggest?
I get so much lately it’s driving me mad so any help
is very much appreciated.
Greetings! Very useful advice within this post! It’s the little changes that make
the most significant changes. Many thanks for sharing!
Ever considering that the casinos began emerging in cities around the
planet, people happen to be looking for tactics to win. They come across this not a challenge
but also a source of passion. And just why don’t you? Playing a casino game stipulates the possibility to getting something for nothing and
there are usually a great deal of individuals eager to fork out cash to find
the best cards or even mixes. Thus, individuals can perform almost anything
to learn to succeed at casino matches.
1 major thing concerning casino games is they are all about probabilities.
That is certainly the reason casino owners insist
on making bets offered to people. In the event
you win then you definitely are able to claim your winnings,
then and if you lose you have to simply take more stakes.
The more stakes you choose from, the larger the losses
you must create. The cut card from roulette and blackjack is just another way to lose.
What exactly is really intriguing about winning casino matches?
Aside from the thrill of rivalry, the adventure of profitable attracts a
particular pride to this man or woman that has pulled
it off. Achieving something through sheer luck or even through some clever plan is a exciting notion. In short, profitable in roulette, blackjack or even any
of another casino matches may offer whoever has attained it enormous pleasure and satisfaction.
Roulette and Texas maintain ’em are two of the absolute most popular video games.
Blackjack and poker are popular. The important thing about these games will be the results is dependent up on the previous two numbers which had been dealt with you, especially, the variety your arms (theces)
and also the range of one’s threes (punches). At the
Texas Hold ’em and the casino version, the successful jackpot,
that will be identified as the flop, is thirtyseven, whilst at the
blackjack variant, it truly is thirty-six.
Nice answers in return of this matter with genuine arguments and describing all on the
topic of that.
I enjoy looking through an article that will make men and women think.
Also, many thanks for permitting me to comment!
Hey! I just wanted to ask if you ever have any problems with
hackers? My last blog (wordpress) was hacked and I ended up losing many months
of hard work due to no back up. Do you have any methods to prevent hackers?
Feel free to surf to my site … hurting traffic
An intriguing discussion is definitely worth comment.
I believe that you ought to publish more on this subject
matter, it might not be a taboo subject but usually folks don’t discuss these issues.
To the next! Best wishes!!
Hello There. I found your blog using msn. This is a
very well written article. I’ll make sure to bookmark it and return to read
more of your useful info. Thanks for the post.
I will definitely return.
Have you ever thought about creating an ebook
or guest authoring on other blogs? I have a blog based upon on the
same ideas you discuss and would really like to have you share
some stories/information. I know my visitors would value
your work. If you’re even remotely interested, feel
free to send me an e mail.
We’re a gaggle of volunteers and opening a brand new scheme in our community.
Your web site provided us with valuable info to work on. You’ve performed a formidable process and
our whole community might be grateful to you.
Thanks on your marvelous posting! I really enjoyed reading it, you may be
a great author.I will make certain to bookmark
your blog and will often come back in the foreseeable future.
I want to encourage you to definitely continue your great posts, have a nice
afternoon!
Yes! Finally something about http://www.autogm.it/index.php?option=com_k2&view=itemlist&task=user&id=2334831.
I really like it when folks get together and share views.
Great website, keep it up!
I am truly glad to glance at this blog posts which carries tons
of helpful data, thanks for providing these statistics.
Great goods from you, man. I have understand your stuff previous to and you’re just extremely
wonderful. I really like what you have acquired here, really like what you’re stating and
the way in which you say it. You make it enjoyable and you still take care of to keep
it sensible. I can’t wait to read far more from you.
This is actually a tremendous web site.
Excellent site you have here but I was curious if you knew of any discussion boards
that cover the same topics discussed here? I’d really like to
be a part of community where I can get comments from other experienced people that share
the same interest. If you have any recommendations, please
let me know. Thanks!
We’re a bunch of volunteers and starting a new scheme in our community.
Your website offered us with useful info to work on. You have performed a formidable task and our whole community
might be thankful to you.
Thanks a lot for sharing this with all people you actually recognise what you’re speaking approximately!
Bookmarked. Kindly also talk over with my website =).
We could have a hyperlink trade agreement among us
Hello Dear, are you truly visiting this website daily, if so
after that you will absolutely take good knowledge.
Hmm it looks like your website ate my first comment (it
was super long) so I guess I’ll just sum it up what I wrote and say, I’m thoroughly enjoying your blog.
I too am an aspiring blog writer but I’m still new to everything.
Do you have any tips and hints for newbie blog
writers? I’d definitely appreciate it.
This design is steller! You definitely know how to keep a reader amused.
Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!) Wonderful job.
I really enjoyed what you had to say, and more than that, how you presented it.
Too cool!
It’s perfect time to make a few plans for the long run and it is time to be
happy. I have learn this submit and if I could I want to recommend you few fascinating things or suggestions.
Perhaps you could write next articles referring
to this article. I wish to read more issues about it!
Some truly nice and utilitarian information on this internet site, too I believe the design and style holds fantastic features.
Review my site; website traffic
Hi there, its fastidious paragraph about media print,
we all be familiar with media is a impressive source of facts.
I have been exploring for a little for any high-quality articles or weblog posts in this kind
of house . Exploring in Yahoo I at last stumbled upon this
web site. Studying this information So i’m glad to convey that I’ve an incredibly good
uncanny feeling I came upon exactly what I needed.
I such a lot surely will make sure to do not overlook this web site and provides it a glance regularly.
http://mpfasdpic.org http://sseinc.org http://constitutionfair.org http://e-oko.com http://evokerc.com http://tajmuseum.com http://promyana-bg.org http://medicalcom.pl http://telesystem.com.pl http://4-bet.com.pl http://pepsiohyesabhi.com http://piszemydlaciebie.pl http://eltying.com.pl http://inclusion-fp7.org http://robobat-polska.pl http://assm2012.pl http://esencjapiekna.com.pl http://cityviewphoto.com http://datasolutions.com.pl http://gosciniecmurckowski.pl http://siteopia.pl http://yourpbc.org http://marriagematterstokids.org http://healthysaulttribe.com http://catapultconsultingsolutions.com http://chuck.com.pl http://healthysaulttribe.comAs I assess the blog sites, I want to pay special focus on the layout
and the key elements on each blog site. Senate Bulk Leader Trent Lott 22
Legislator Lott, at a celebration recognizing Adding a catchy phrase or line, describing the nature of your
blog is useful too.
It’s appropriate time to make some plans for the
longer term and it’s time to be happy. I’ve learn this publish and if I could I want
to suggest you some fascinating things or suggestions.
Maybe you can write next articles regarding this article.
I want to read more issues approximately it!
https://Tinyurl.com/nv8efzbm https://cutt.ly/xTQzjTP https://tinyurl.com/cmyx8zsw https://www.Wieczniezaczytana.pl/ https://dressage.pl https://pasowaniesiodel.pl https://cutt.ly/FTQzhuH https://cutt.ly/MTQl5PN https://Whattodo.com.pl/ https://cutt.ly/OTQzxrd https://pasowaniesiodel.pl https://yard-equites.pl https://bit.ly/30BGVO1 https://bit.ly/3kN0wl5 https://tinyurl.com/bax3b49t https://Tinyurl.com/yxaympc7 https://equitrend.pl https://oficerki.pl https://bit.ly/30HDF3z https://whattodo.com.pl https://tinyurl.com/n9eja6ud
An intriguing discussion is definitely worth comment. There’s no doubt that that you
need to publish more on this subject, it may not be a taboo matter but generally
folks don’t talk about such issues. To the next! Kind regards!!
Wow, that’s what I was exploring for, what a data! existing
here at this blog, thanks admin of this web page.
https://cutt.ly/gUTSB2g https://bit.ly/3b1KIpt http://ubezpieczenie-dziecka.pl https://Bit.ly/34aKa0n https://cutt.ly/MRQM6Ph http://ubezpieczenia-bydgoszcz.net.pl https://bit.ly/3B6ly3t https://bit.ly/3eExRvf https://cutt.ly/LUTDr1X http://glowackiubezpieczenia.pl https://tinyurl.com/v3rytj3s https://cutt.ly/sRAzgRD https://cutt.ly/TRQMNcO https://tinyurl.com/7tkv79cb https://bit.ly/34aKa0n https://Cutt.ly/TRQMNcO https://Cutt.ly/yUTDxPS http://noweubezpieczenia.pl http://ubezpieczenia-bydgoszcz.net.pl http://ubezpieczenialekarskie.pl https://tinyurl.com/ybb4tr3y
Hello! I’ve been following your web site for a
while now and finally got the courage to go ahead and give you a shout out
from Dallas Texas! Just wanted to tell you keep up the
great work!
I visit everyday some sites and sites to read articles,
however this webpage gives feature based writing.
Keep this going please, great job!
After looking at a number of the articles on your blog, I truly like your way
of writing a blog. I added it to my bookmark site list and will be checking back soon.
Please check out my website as well and let me know how you
feel.
I all the time used to read piece of writing in news papers but
now as I am a user of web thus from now I am using net for posts, thanks to web.
Howdy! Someone in my Myspace group shared this site with us so I came to look it over.
I’m definitely loving the information. I’m book-marking and will be tweeting
this to my followers! Wonderful blog and excellent style and design.
Great work! This is the kind of information that are supposed to be shared around the net.
Disgrace on Google for not positioning this submit higher!
Come on over and consult with my website . Thank you =)
Heya i am for the primary time here. I found this board
and I to find It truly useful & it helped me out a lot.
I’m hoping to offer one thing again and help others such as
you aided me.
It’s wonderful that you are getting thoughts from this article as well
as from our discussion made at this place.
Hi there, You’ve done an excellent job. I’ll certainly digg
it and personally recommend to my friends. I’m sure they’ll be benefited from this site.
Wonderful work! This is the type of information that are supposed
to be shared around the net. Disgrace on the seek engines for now not positioning this post upper!
Come on over and consult with my website . Thank
you =)
you’re in reality a excellent webmaster. The site loading pace is
amazing. It seems that you are doing any unique trick.
Furthermore, The contents are masterpiece. you have performed a
fantastic process on this matter!
It is perfect time to make some plans for the future and it is time to be happy.
I’ve read this post and if I could I wish to suggest you few interesting things
or advice. Perhaps you can write next articles referring to this article.
I desire to read more things about it!
Write more, thats all I have to say. Literally, it seems as
though you relied on the video to make your point. You clearly know what
youre talking about, why throw away your intelligence on just posting
videos to your site when you could be giving us something
informative to read?
check this link right here now
jaxx web wallet
I’m really enjoying the theme/design of your website.
Do you ever run into any web browser compatibility issues? A few of my blog visitors have complained about
my site not working correctly in Explorer but looks great in Firefox.
Do you have any suggestions to help fix this issue?
Hi! I’ve been following your weblog for some time now and finally got the courage to go ahead and give you a
shout out from Huffman Texas! Just wanted to tell you keep up the fantastic
job!
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added I get four e-mails with
the same comment. Is there any way you can remove people from that
service? Bless you!
Thanks , I’ve recently been searching for info about this subject for a while and yours is the best
I’ve found out till now. But, what about the bottom line?
Are you certain concerning the supply?
I’m truly enjoying the design and layout of your site. It’s a very
easy on the eyes which makes it much more enjoyable for me to come here and visit more often.
Did you hire out a developer to create your theme?
Superb work!
Greetings from Florida! I’m bored at work so I decided to check out your site on my iphone during lunch break.
I love the knowledge you provide here and can’t wait to take a look when I get home.
I’m shocked at how quick your blog loaded on my phone ..
I’m not even using WIFI, just 3G .. Anyhow,
great site!
This design is wicked! You definitely know how to keep a reader entertained.
Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!) Fantastic
job. I really loved what you had to say, and more than that, how
you presented it. Too cool!
Hi, I do think this is a great site. I stumbledupon it 😉 I will return yet again since i have book marked it.
Money and freedom is the best way to change, may you be rich and continue
to help others.
find this Pirate Story by Robert Louis Stevenson
I am really grateful to the holder of this web page
who has shared this enormous post at at this time.
Your way of describing everything in this paragraph is truly good, every one be able
to without difficulty understand it, Thanks a lot.
hello!,I love your writing very a lot! proportion we communicate extra about your article on AOL?
I require an expert on this area to solve my problem.
Maybe that is you! Having a look ahead to look you.
Do you have a spam problem on this website; I also am a
blogger, and I was wondering your situation; many of us have created some nice procedures and we are looking
to trade methods with other folks, why not shoot
me an e-mail if interested.
I am curious to find out what blog system you have been utilizing?
I’m experiencing some small security problems with my latest blog and I’d like to find something more safe.
Do you have any suggestions?
Very good article. I’m dealing with many of these issues
as well..
Please let me know if you’re looking for a article author for your site.
You have some really great posts and I believe I would be a good asset.
If you ever want to take some of the load off, I’d love to write some content for your blog
in exchange for a link back to mine. Please send me an email if interested.
Regards!
Nice blog! Is your theme custom made or did you download
it from somewhere? A design like yours with a few
simple adjustements would really make my blog shine. Please let me know
where you got your design. Kudos
What’s Going down i am new to this, I stumbled
upon this I’ve discovered It absolutely helpful and it has helped me out loads.
I’m hoping to contribute & aid different customers like its aided me.
Great job.
This definitely be the next preference. You are perfect, theme team. I Really enjoy the system, fonts along with the perfect subject. Thanks for a great valuable design. Great job!